Understanding Chemical Peels and Lasers for Skin Texture Concerns
Chemical peels and laser treatments both aim to improve skin texture, but they do so through fundamentally different mechanisms. Chemical peels exfoliate the skin to promote renewal, whereas lasers use energy to stimulate collagen production and remodel the skin’s structure. Because they target different layers of the skin, neither option is universally superior.
The right choice depends on several factors, including the severity of texture irregularities, the specific skin concerns (e.g., acne scarring, enlarged pores, dullness, or pigmentation), and an individual’s tolerance for downtime and skin type. This article explains how chemical peels and laser treatments differ with respect to mechanism, applications, recovery, safety, and cost, helping readers determine which approach is more appropriate for different texture concerns.
What Does Skin Texture Mean?
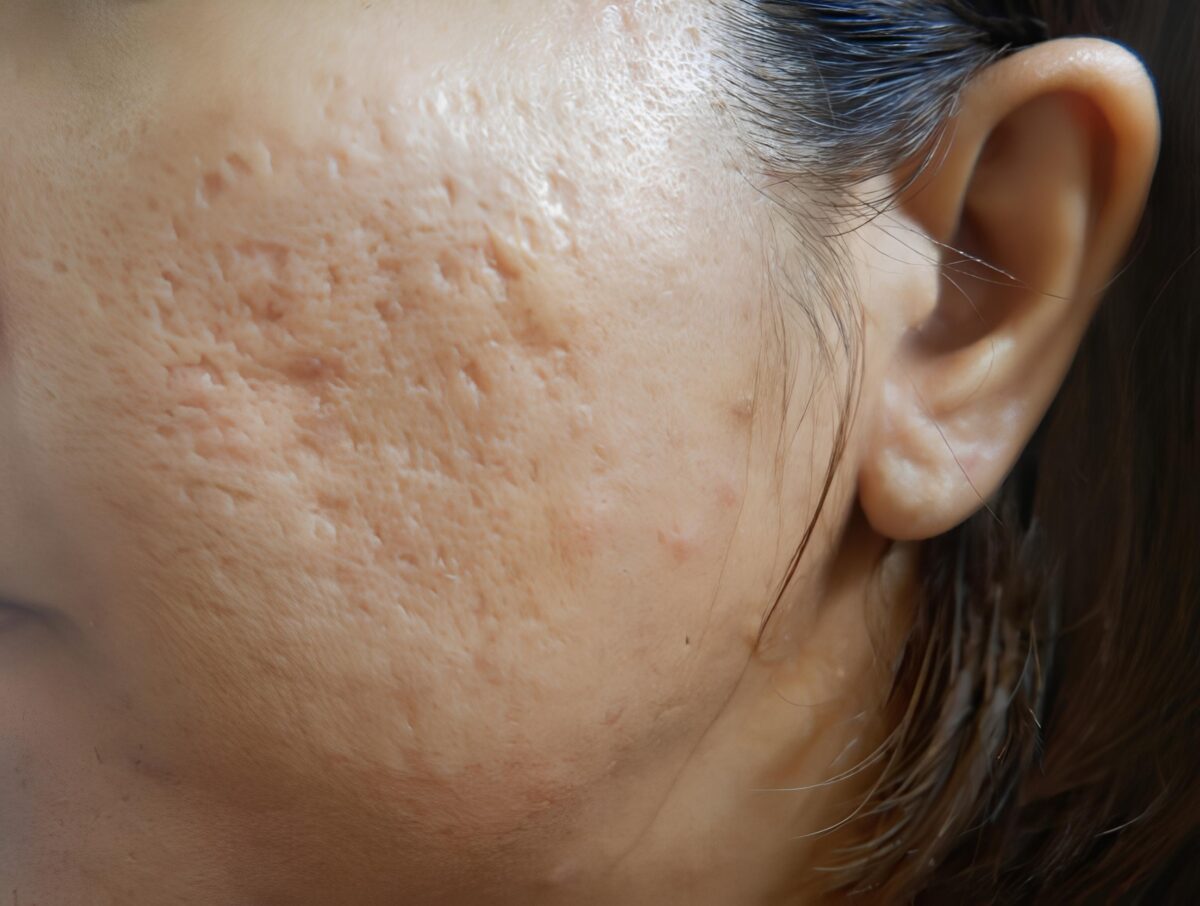
In dermatology, skin texture refers to the smoothness, evenness, and uniformity of the skin surface. Texture concerns are common and can arise from acne, ageing, sun exposure, or inflammation. These issues vary in depth; therefore, treatment selection depends on whether the problem is superficial or structural.
Common skin texture issues include roughness, in which the skin feels coarse or uneven to the touch, and an uneven surface, in which light reflects irregularly due to textural changes. Enlarged pores can also contribute to an uneven texture by disrupting the skin’s smooth appearance. In addition, fine acne scarring, such as shallow atrophic scars, can subtly alter skin texture even when deeper scars are absent.
It is important to distinguish between surface-level texture issues and deeper structural texture changes. Surface-level concerns affect the outermost layers of the skin and often respond well to exfoliation-based treatments. Deeper texture changes involve collagen loss or dermal damage and typically require treatments that stimulate collagen remodelling. This distinction explains why chemical peels and laser treatments are used differently and cannot be interchanged.
How Chemical Peels Improve Skin Texture
Chemical peels remove damaged superficial layers of the skin in a controlled manner to help address surface irregularities. By accelerating exfoliation and renewal, peels help smooth roughness, even out tone, and refine mild textural irregularities that originate near the skin surface.
What Are Chemical Peels?
Chemical peels are dermatologic treatments that use controlled exfoliation to support surface skin renewal. A chemical solution is applied to the skin to break the bonds between old skin cells, thereby removing superficial skin layers and stimulating regeneration. The depth of exfoliation depends on the type and concentration of the peeling agent used.
How Chemical Peels Work
Chemical peels work by encouraging natural exfoliation, allowing new, healthier skin cells to replace damaged ones more quickly. This process encourages surface renewal, which can help address dullness and surface irregularities.
Depending on the depth of peel, chemical peels can also induce mild collagen stimulation, particularly with medium-depth formulations. As their primary effects are surface-focused, chemical peels are generally used for superficial texture concerns rather than deeper structural issues.
Types of Chemical Peels (High Level)
- Superficial peels act on the outermost skin layer and are commonly used for roughness, dullness, and mild uneven texture. Downtime is minimal.
- Medium-depth peels penetrate deeper and can improve more noticeable texture irregularities, but require longer recovery.
- Deep peels reach the lower dermal layers and carry a higher risk. They are used selectively and require careful patient selection and medical supervision.
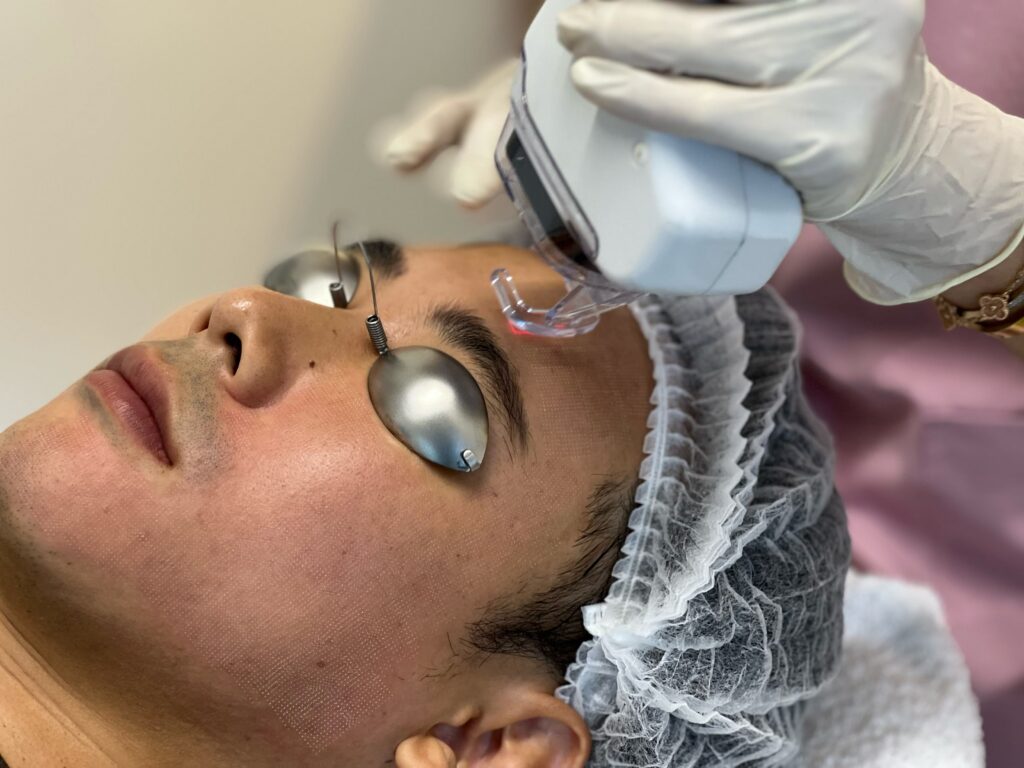
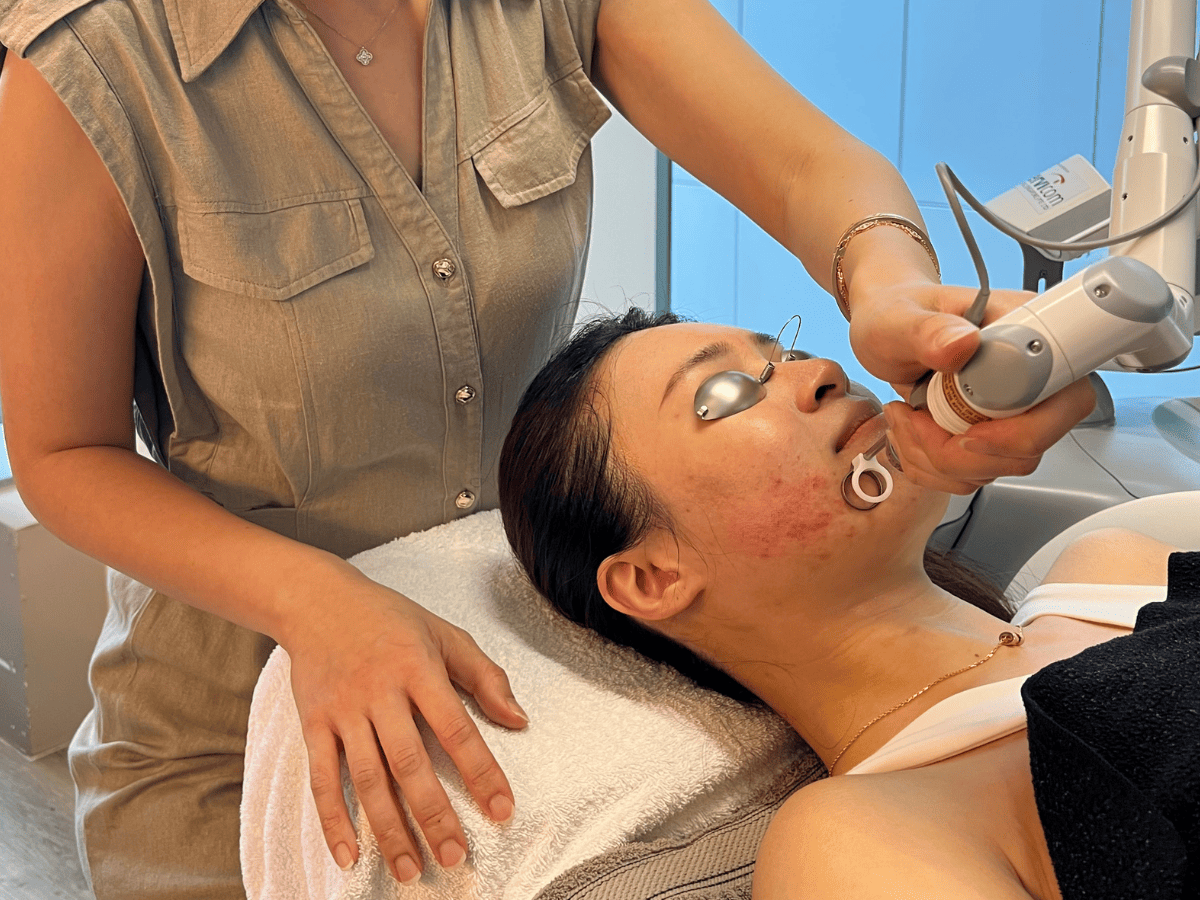
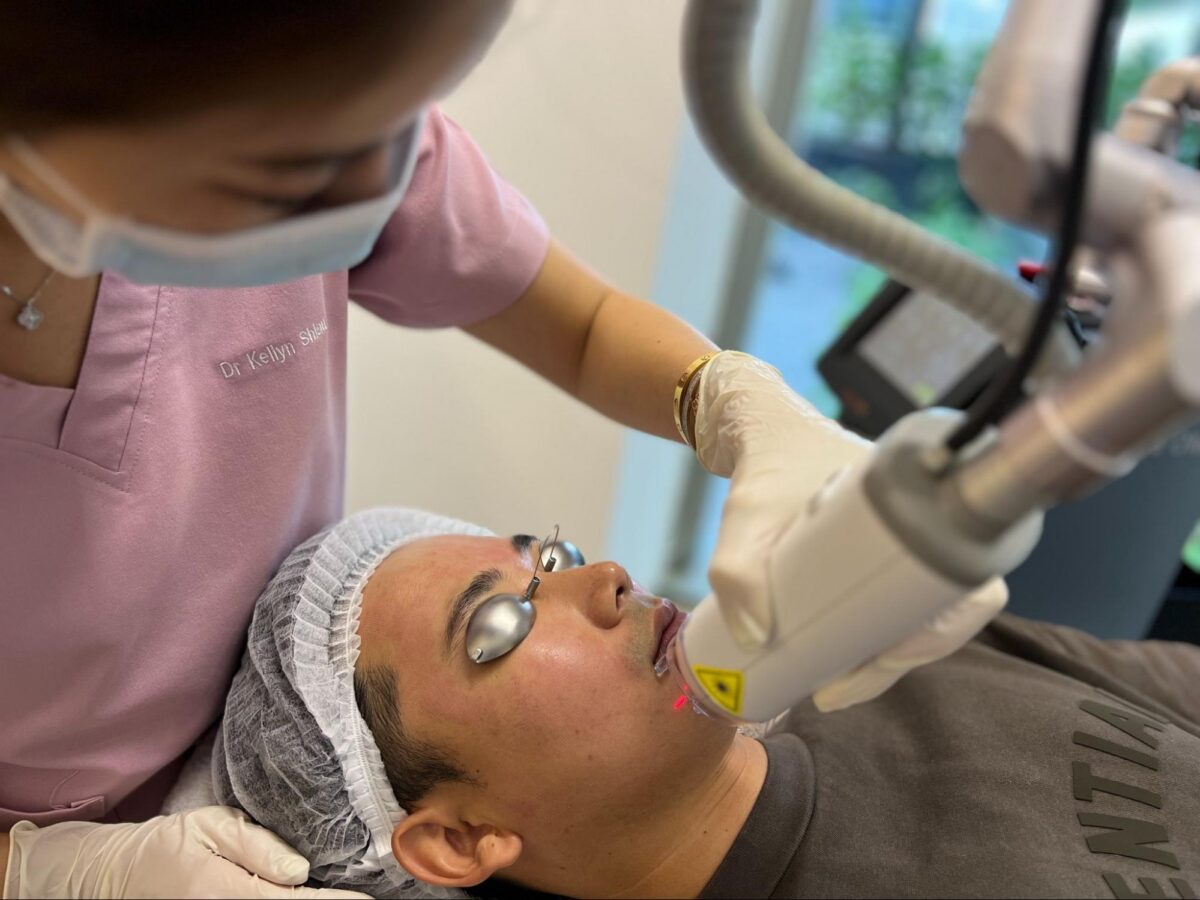
How Laser Treatments Improve Skin Texture
Laser treatments improve skin texture by delivering targeted energy to stimulate collagen production and remodel the skin’s structure. Unlike chemical peels, lasers can address both surface and deeper dermal layers, depending on the technology used.
What Is Laser Treatment for Skin Texture?
Laser treatment for skin texture is an energy-based approach that delivers controlled laser energy to the skin. This energy can target the skin surface, the dermis, or both, making lasers more versatile for a wider range of texture concerns, including those caused by collagen loss.
How Laser Treatment Works
Lasers improve texture primarily by stimulating collagen production, triggering the skin’s natural repair process to strengthen and smooth the dermal framework. Some lasers also perform resurfacing, removing damaged tissue to create a smoother surface.
Laser approaches are broadly divided into:
- Ablative lasers, which remove microscopic columns of skin and induce strong collagen remodelling
- Non-ablative lasers, which leave the surface intact while stimulating collagen beneath the skin
This distinction explains why lasers can treat deeper texture irregularities that chemical peels cannot.
Chemical Peels and Laser Key Differences
The table below summarises the differences between chemical peels and laser treatments in mechanism, depth, effectiveness, and recovery. This comparison highlights why these treatments are not interchangeable, but instead suited to different texture concerns.
| Comparison Dimension | Chemical Peels | Laser Treatments |
|---|---|---|
| Mechanism of action | Chemical exfoliation | Energy-based collagen stimulation |
| Depth of treatment | Primarily superficial | Surface and/or dermal layers |
| Best texture concerns addressed | Roughness, dullness, mild uneven texture | Deeper texture irregularities, pores, and acne-related texture |
| Speed of visible improvement | Gradual, over repeated peels | Often faster per session |
| Number of sessions required | Multiple sessions are common | Fewer sessions |
| Downtime and recovery | Minimal to moderate, depending on peel depth | Ranges from minimal to several days |
| Safety across skin types | Depends on peel type and depth | Depends on laser type and settings |
| Typical cost positioning | Lower per session | Higher per session |
Which Works Better for Different Skin Texture Concerns?
Chemical peels and laser treatments target different types of skin texture concerns as they act at varying skin depths. A medical assessment can help determine whether a skin texture concern is superficial or involves deeper layers, which may influence the choice of treatment.
Mild Roughness and Dull Skin
Chemical peels perform particularly well for mild roughness and dull-looking skin. These concerns usually originate from the accumulation of dead skin cells on the surface, which interferes with light reflection and smoothness.
Superficial chemical peels help by exfoliating the outermost layer of the skin, which can help improve the look of dull or uneven skin over time. For patients whose primary concern is surface roughness rather than scarring or enlarged pores, chemical peels are often sufficient and cost-effective.
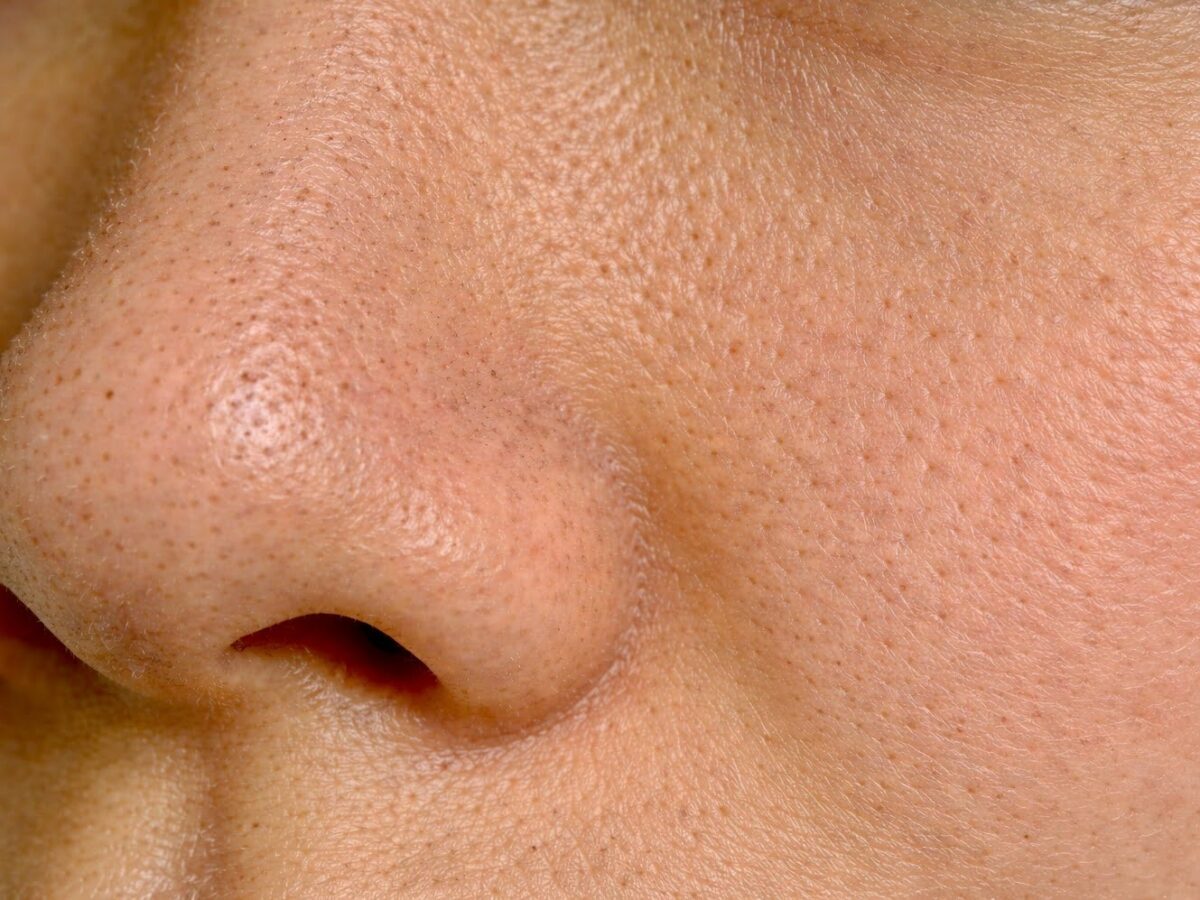
Enlarged Pores and Uneven Texture
Lasers are commonly used in the management of enlarged pores and uneven skin texture. These concerns are often associated with collagen weakness around the pores or with irregularities in the dermal structure.
Chemical peels may help improve surface smoothness. However, when concerns are related to deeper collagen changes, other treatments such as lasers may also be considered. Laser treatments stimulate collagen remodelling, which can tighten surrounding tissue and improve overall texture, which may not be consistently achieved with peels.
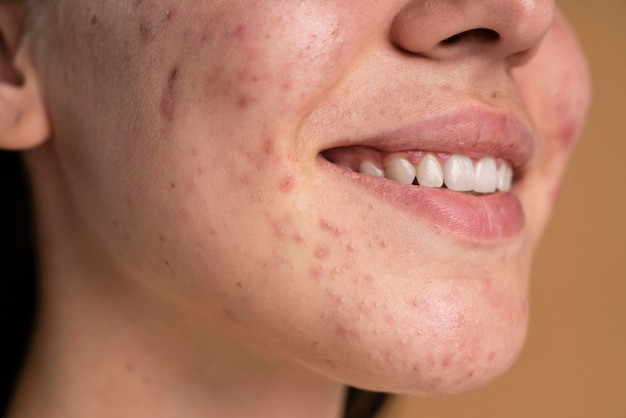
Acne-Related Texture Irregularities
Acne-related texture irregularities vary in depth, which affects treatment response.
- Shallow texture changes, such as fine irregularities left after acne, may improve with repeated chemical peels.
- Deeper textural changes, including shallow scars or uneven dermal architecture, respond more effectively to laser treatments.
For this reason, lasers often outperform chemical peels when texture irregularities are related to acne scarring, particularly when collagen loss is involved.
Safety and Skin Type Considerations
Safety is an important consideration when choosing between chemical peels and lasers, particularly for patients prone to pigmentation issues.
Chemical peels carry a risk of irritation and post-inflammatory hyperpigmentation (PIH), especially when stronger peels are used or when aftercare is inadequate. The risk increases with deeper peels and in darker skin types.
Laser safety varies depending on the type of laser and the settings used. Certain laser technologies are suitable across a wide range of Fitzpatrick skin types, while others require more caution in darker skin due to PIH risk.
In both cases, proper treatment depth, conservative settings, and appropriate aftercare are critical. Provider experience plays a key role in minimising complications and selecting the most appropriate treatment for each skin type.
Cost Considerations — Peels vs Laser
Chemical peels are generally lower in cost per session, but they often require more frequent treatments to maintain results. They are well suited for ongoing maintenance and superficial concerns. Laser treatments typically have a higher per-session cost, but fewer sessions may be needed to achieve noticeable improvement, particularly for deeper texture issues.
As a result, total cost depends less on the price of a single session and more on treatment goals, depth of concern, and the number of sessions required over time.
Can Chemical Peels and Lasers Be Combined?
Combination approaches are common because chemical peels and lasers address different layers of the skin.
A typical strategy involves:
- Chemical peels for surface refinement, brightness, and maintenance
- Laser treatments for deeper texture improvement and collagen remodelling
This sequencing allows surface issues to be addressed while reserving lasers for concerns that require deeper intervention. From a cost-effectiveness perspective, combination treatment can produce more balanced and longer-lasting results, reducing the need for repeated ineffective treatments.
FAQs
Are chemical peels enough for uneven skin texture?
Chemical peels are effective for surface-level texture issues but may be insufficient for deeper structural irregularities.
Do lasers work better for acne-related texture?
Yes. Lasers generally work better when texture irregularities are related to collagen loss or acne scarring.
Which option has less downtime?
Chemical peels usually involve less downtime, especially superficial peels, while laser downtime varies by type.
Can peels replace laser treatment completely?
No. Chemical peels cannot fully replace lasers for deeper texture concerns that require collagen remodelling.