Understanding Wrinkles: Causes, Symptoms, 4 Treatments and More
Wrinkles are a natural part of ageing. These lines and folds in the skin appear as collagen and elastin gradually break down over time. While wrinkles are a normal change in the skin, some individuals may explore ways to support skin health and maintain its appearance.
What Are Wrinkles?
Wrinkles are creases or lines that form on the skin’s surface. It develops due to both intrinsic (biological) and extrinsic (environmental) factors. Over time, these factors weaken the skin’s structure and it loses its elasticity, making it thinner and less able to retain moisture. This process, along with repeated facial expressions, causes the skin to sag and fold, forming wrinkles.
Types of Wrinkles
Wrinkles are generally classified into three main types:
| Type of Wrinkle | Description | Severity Level |
|---|---|---|
| Dynamic Wrinkles | Formed by facial movements; visible during expressions | Mild to Moderate |
| Static Wrinkles | Always present; deepens with age | Moderate to Severe |
| Wrinkle Folds | Deep grooves due to sagging skin | Severe |
1. Dynamic Wrinkles
These form from repeated facial movements, like smiling or frowning. They usually appear around areas with high muscle activity, such as the forehead and around the eyes. While they’re initially visible only when you make expressions, over time, they may become permanent.
2. Static Wrinkles
Static wrinkles are visible even when your face is relaxed. They occur due to a loss of skin elasticity and are more prominent as skin thins with age. These wrinkles are usually found in areas like the cheeks and neck.
3. Wrinkle Folds
These deeper lines are caused by the sagging of the skin, often from the nose to the corners of the mouth.
The percentage of developing these types of wrinkles varies by age:
| Age Group | Dynamic Wrinkles (%) | Static Wrinkles (%) | Wrinkle Folds (%) |
|---|---|---|---|
| 20s | 10 | 5 | 0 |
| 30s | 30 | 15 | 5 |
| 40s | 50 | 30 | 20 |
| 50s+ | 70 | 50 | 40 |
Common areas with wrinkles/lines
Wrinkles can form in various areas of the face and body, including:
- Forehead lines
- Under-eye wrinkles
- Crow’s feet
- Nasolabial folds
- Marionette lines
- Neck wrinkles
- Chest wrinkles
- Hand wrinkles
Causes of Wrinkles
Wrinkles develop due to ageing and genetics, sun exposure and UV damage, lifestyle factors and repeated facial movements.
Ageing and Genetics
As we age, our skin undergoes changes that lead to wrinkles. Collagen and elastin production, essential proteins for skin’s elasticity and structure, decrease over time. This reduction results in thinning skin, loss of moisture, and the formation of lines and creases.
Genetic predisposition also plays a significant role; individuals with a family history of early wrinkling are more likely to develop wrinkles themselves.
Sun Exposure and UV Damage
Prolonged exposure to the sun’s ultraviolet (UV) radiation is a common cause of premature skin ageing, known as photoaging. It breaks down collagen and elastin fibres in the skin, leading to wrinkles.
Lifestyle Factors
Lifestyle can significantly affect skin health and wrinkle development. Smoking can reduce the blood flow to the skin, depriving it of nutrients and oxygen, which accelerates ageing. Additionally, poor diet, lack of sleep, dehydration, and high-stress levels can contribute to premature wrinkling.
Repeated Facial Movements
Frequent facial expressions, such as frowning or squinting, contribute to dynamic wrinkles. Over time, these movements create permanent lines in the skin.
Symptoms and Diagnosis of Wrinkles
The main symptom of wrinkles is the presence of fine lines, creases, or folds on the skin. Wrinkles can vary in severity, ranging from mild to severe. Doctors may assess wrinkle severity through clinical examination and non-invasive skin analysis.
- Mild: Fine lines that are barely noticeable.
- Moderate: Visible lines and slight sagging.
- Severe: Deep creases and significant skin sagging.
Treatment Options for Wrinkles
Wrinkle treatments range from topical treatments to cosmetic procedures and advanced medical treatments.
- Topical Treatments
Topical treatments like retinoids, peptides, and antioxidants work by stimulating collagen production and promoting cell turnover. These are commonly used to improve the appearance of wrinkles and skin texture.
| Topical Treatment | Description | Effectiveness for Wrinkles | Key Ingredients | Side Effects |
|---|---|---|---|---|
| Retinoids | Vitamin A derivatives that promote cell turnover and collagen production. | Highly effective in reducing fine lines and improving skin texture; results can be seen within a few weeks to months. | Tretinoin, Adapalene, Retinaldehyde | Redness, peeling, dryness, and irritation, especially at the beginning of use. |
| Peptides | Short chains of amino acids that help stimulate collagen production and improve skin elasticity. | Moderately effective; results are gradual and may take several weeks to months to become noticeable. | Palmitoyl pentapeptide-4, Acetyl hexapeptide-8 | Generally well-tolerated; minimal side effects like mild irritation or allergic reactions. |
| Antioxidants | Compounds that protect the skin from oxidative stress and environmental damage. | Effective in preventing further wrinkle formation and improving overall skin appearance; results vary based on formulation. | Vitamin C, Vitamin E, Coenzyme Q10 | Rarely cause side effects; may cause mild irritation in sensitive skin types. |
- Cosmetic Procedures
Non-invasive cosmetic procedures (dermal fillers and chemical peels) are used to target specific types of wrinkles
| Treatment | Pros | Cons |
|---|---|---|
| Botox |
– Quick procedure with minimal downtime. – Effectively reduces dynamic wrinkles by relaxing facial muscles. – Can prevent new wrinkles from forming when used regularly. |
– Temporary results lasting 3–6 months; requires repeat treatments. – Possible side effects include bruising, headaches, and drooping. – Requires skilled administration to avoid complications. |
| Dermal Fillers |
– Immediate results in restoring volume and smoothing wrinkles. – Can enhance facial contours and improve overall appearance. – Minimal downtime; most patients resume normal activities quickly. |
– Results vary based on the type of filler used; may last 6–18 months. – Risk of swelling, bruising, or allergic reactions at injection sites. – Potential for lumpiness or uneven results if not properly injected. |
| Chemical Peels |
– Improves skin texture and tone by removing dead skin cells. – Can reduce fine lines and sun damage effectively. |
– Recovery time varies; redness and peeling can last several days. – Risk of irritation, scarring, or changes in skin pigmentation. |
- Advanced Medical Treatments
Medical procedures like laser therapy, microneedling, and radiofrequency may help improve skin texture and support collagen production. They are commonly used in cases involving deeper wrinkles
| Treatment | Benefits | Risks |
|---|---|---|
| Laser Therapy |
– Stimulates collagen production, leading to smoother skin. – Can target specific areas and improve skin tone and texture. – Minimal downtime; most patients return to normal activities quickly. |
– Possible side effects include redness, swelling, and discomfort. – Risk of pigmentation changes, especially in darker skin tones. – Requires skilled practitioners to avoid complications. |
| Microneedling |
– Enhances skin texture and firmness by promoting collagen production. – Can improve the appearance of scars and stretch marks in addition to wrinkles. – Minimal downtime; patients can usually resume normal activities shortly after treatment. |
– Temporary redness and swelling. – Risk of infection if not done properly. – Results may take time to appear and require patience. – Not suitable for all skin types; professional assessment is required. |
| Radiofrequency |
– Non-invasive treatment that tightens skin and reduces wrinkles. – Stimulates collagen production with little to no downtime. – Safe for various skin types and can be combined with other treatments. |
– Possible redness, swelling, or discomfort at the treatment site. – Results can vary depending on individual skin type and condition. – Results may not be permanent. |
Preventing Wrinkles
Preventing wrinkles includes daily skincare routines, sun protection strategies, and lifestyle modifications. Here are some helpful tips:
Daily Skin Care Routines
A consistent skincare routine tailored for wrinkle prevention is vital. Here’s a step-by-step guide:
- Use a gentle cleanser twice a day. Start with a gentle cleanser to remove dirt without stripping the skin’s natural oils.
- Apply a toner. Use a hydrating toner to balance the skin’s pH for subsequent products.
- Nourish your skin with some serum. Apply a serum containing antioxidants (like Vitamin C) to protect against environmental damage and promote collagen production.
- Moisturise. Choose a moisturiser rich in hyaluronic acid or peptides to hydrate and plump the skin.
- Apply some eye cream. Use a product specifically formulated to target fine lines and puffiness around the delicate eye area.
Sun Protection Strategies
Sun protection helps prevent premature ageing and wrinkles. Here’s a comparison of different broad-spectrum sunscreen products:
| Product Type | SPF Level | Broad-Spectrum Protection | Water Resistance | Recommended Use |
|---|---|---|---|---|
| Sunscreen Lotion | SPF 30–50 | Yes | 40–80 minutes | Daily use on all exposed skin |
| Sunscreen Spray | SPF 30–50 | Yes | 40–80 minutes | Convenient for reapplication |
| Sunscreen Stick | SPF 30–50 | Yes | Not applicable | Ideal for sensitive areas (e.g., face) |
| Moisturiser with SPF | SPF 15–30 | Yes | Varies | Daily use as part of skincare routine |
Lifestyle Modifications
In addition to skincare, changes in your lifestyle can support skin health and help prevent wrinkles. Here are some things you can do:
- Stay hydrated. Drink enough water to keep your skin hydrated from within.
- Eat a balanced diet. Incorporate fruits, vegetables, healthy fats and lean proteins to provide essential nutrients for skin health.
- Get enough sleep. Aim for 7 to 9 hours of deep sleep every night to allow your skin to repair and regenerate.
- Avoid smoking. Smoking accelerates skin ageing and contributes to wrinkle formation; quitting cigarettes and electronic cigarettes can help prevent premature facial wrinkling.
- Limit alcohol consumption. Excessive alcohol can dehydrate the skin. If you have to drink, make sure to do it in moderation.
- Manage stress. Practice activities like meditation or yoga to reduce stress and help maintain overall skin health.
Comparing Wrinkles with Other Signs of Skin Aging
Wrinkles are sometimes associated with fine lines and age spots. Here’s how they differ:
Wrinkles vs. Fine Lines
Fine lines are often the early stage of wrinkles, appearing as small, shallow creases. Wrinkles are more noticeable and can deepen over time.
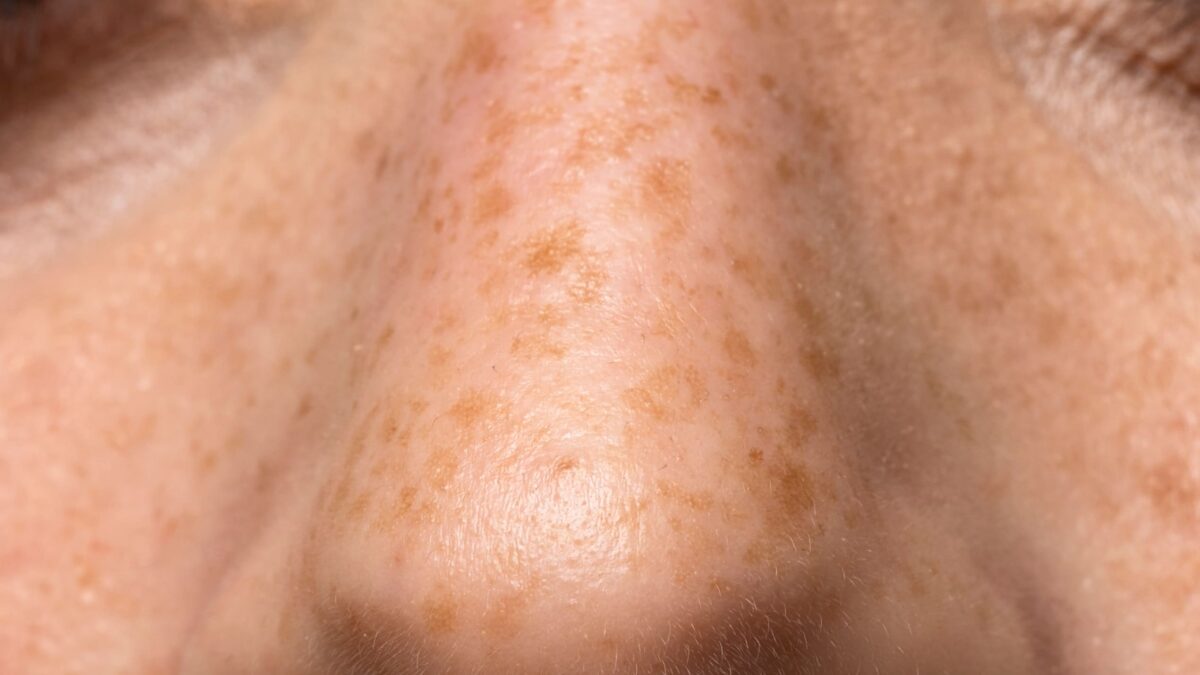
Wrinkles vs. Age Spots
While wrinkles result from a loss of skin elasticity, age spots are caused by an overproduction of melanin, often due to sun exposure. They appear as small, dark patches on the skin.
When to See a Doctor
If you’re concerned about changes in your skin or the appearance of wrinkles, it may be helpful to consult a doctor. They can provide a professional assessment and guide you on possible next steps for skin management.
Conclusion
Understanding wrinkle causes, symptoms, and treatment options is essential for maintaining healthy skin. By adopting a skincare routine, protecting your skin from UV damage, and making healthy lifestyle choices, you can support skin health and help minimise the visible effects of ageing over time.