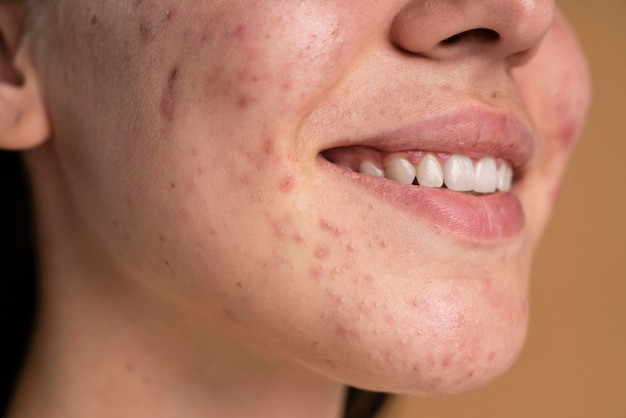
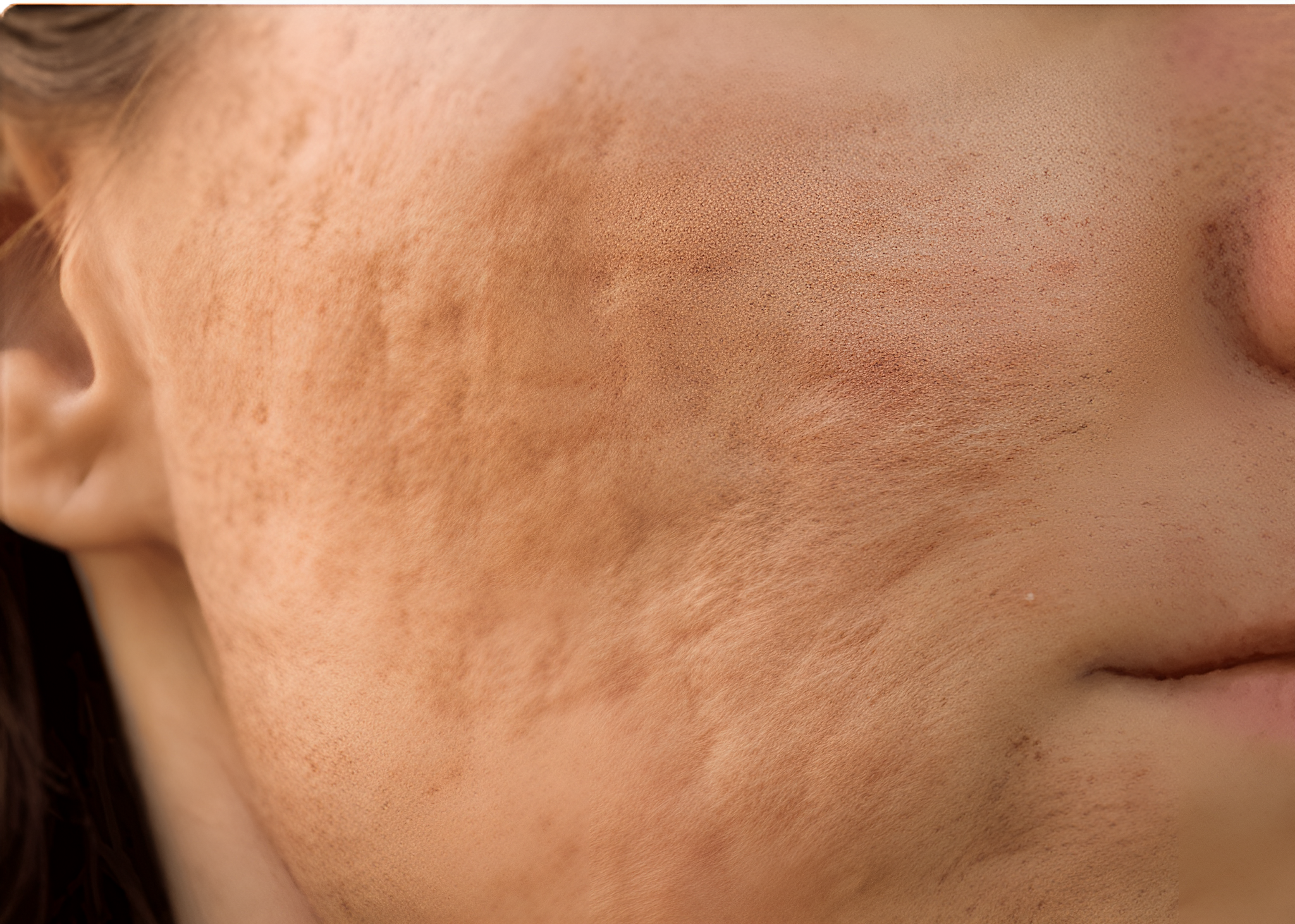
Atrophic acne scars often result from collagen loss and dermal disruption. When the skin is unable to regenerate normal collagen after acne-related inflammation, depressions persist, resulting in permanent textural changes. Subcision and microneedling are two commonly used acne scar treatments that work through different biological pathways to support the skin’s own collagen production.
Subcision works by creating controlled injury beneath the scar to release tethering and trigger collagen production from below. Microneedling, on the other hand, creates numerous micro-injuries in the dermis to stimulate more widespread collagen renewal. Both rely on the skin’s natural healing process but act at different depths and through distinct mechanisms.
Why Collagen Loss Causes Acne Scars
Atrophic acne scars develop when inflammation damages the dermal matrix, and the skin fails to regenerate normal collagen during healing. Two related changes occur: loss of dermal collagen and the formation of disorganised scar collagen. Normal skin relies on a dense, well-organised collagen network to maintain structural support. When acne disrupts this framework, the overlying skin loses its foundation and collapses inward. This is why acne scars often appear indented: the skin lacks the underlying support necessary to remain even.
A key objective in acne scar treatment is to stimulate collagen neogenesis, new, well-organised collagen that helps restore support beneath the scar. Treatments that successfully stimulate collagen neogenesis can gradually improve scar appearance and overall skin texture.
How the Skin Produces New Collagen After Injury
When the skin is injured, it undergoes a natural healing process involving four stages: hemostasis, inflammation, tissue growth, and remodelling. Early in the healing process, the body produces a temporary form of collagen (Type III), which is later replaced by stronger, more organised collagen (Type I). This process is driven by fibroblasts and growth factors that are activated during inflammation. Over time, the new collagen helps restore structure in the skin, improving strength and texture.
Some acne scar treatments aim to support this process by triggering controlled injury that restarts collagen production in targeted areas, a method often referred to as percutaneous collagen induction.
How Subcision Stimulates Collagen Production
Subcision stimulates collagen production by creating a controlled injury in the deep dermis, thereby releasing scar tethering and initiating a prolonged wound-healing response.
Mechanical Release of Fibrous Scar Bands
Many atrophic acne scars are held down by fibrous bands that connect the dermis to deeper tissues. During Subcision, a specialised needle is used to cut these bands beneath the scar. This release can cause the scar to lift visibly, but this immediate improvement represents only part of the treatment effect. The more important long-term benefit comes from the biological response that follows the controlled injury.
Controlled Deep Dermal Injury and Collagen Filling
When fibrous bands are released, Subcision creates a subdermal wound pocket beneath the scar. This space fills with blood, forming a clot that acts as a temporary scaffold.
Within this scaffold, fibroblasts migrate into the wound space and begin depositing new collagen as part of the healing process. This newly formed collagen gradually occupies the space created by Subcision, replacing the void with structural dermal support rather than allowing the scar to re-tether.
Long-Term Collagen Remodelling After Subcision
Collagen formation continues for several months. Initial repair collagen is gradually remodelled into stronger, more organised collagen that integrates with the surrounding tissue. As a result, the scar is no longer anchored, and the results are often long-lasting, especially when Subcision is combined with other treatments that enhance dermal quality.
How Microneedling Stimulates Collagen Production
Microneedling promotes collagen production by creating controlled micro-injuries across the dermis. Unlike Subcision, it doesn’t target individual scars but stimulates collagen renewal across a broader area.
Controlled Micro-Injuries in the Dermis
During microneedling, multiple fine needles create thousands of microscopic punctures in the skin. These micro-channels extend into the dermis while causing minimal disruption to the epidermis.
Because the surface barrier remains largely intact, microneedling induces a controlled injury sufficient to initiate healing without significant inflammation or downtime. This makes it suitable for repeated treatments and for patients at higher risk of pigmentation.
Growth Factor Release and Fibroblast Activation
The micro-injuries activate platelets and cytokines, which release growth factors that stimulate fibroblasts. This initiates the formation of new collagen and blood vessels throughout the treated skin.
Rather than filling a discrete wound pocket as in Subcision, microneedling stimulates widespread collagen production throughout the treated dermis. This results in the gradual thickening of the dermal layer and improved collagen organisation over time.
Gradual Dermal Thickening and Scar Softening
Collagen deposition following microneedling is incremental, occurring over weeks to months with repeated treatments. Instead of immediate scar elevation, patients typically notice progressive softening of scars and a smoother texture. Microneedling doesn’t mechanically lift scars, but it improves the skin’s overall quality and texture, especially when used as part of a comprehensive treatment plan.
Subcision and Microneedling Collagen Stimulation
The table below summarises how Subcision and microneedling stimulate collagen through different biological pathways, highlighting why they are complementary rather than interchangeable.
| Comparison Dimension | Subcision | Microneedling |
|---|---|---|
| Type of injury | Mechanical release and deep dermal injury | Repeated micro-injury |
| Depth of collagen stimulation | Deep dermis and subdermal plane | Superficial to mid-dermis |
| Speed of visible improvement | Immediate partial lift with gradual improvement | Gradual improvement only |
| Type of collagen response | Focal collagen filling and structural support | Diffuse collagen thickening |
| Suited scar types | Tethered rolling and boxcar scars | Shallow, diffuse atrophic scars |
| Longevity of collagen changes | Often long-lasting | Maintained with repeated sessions and ongoing care |
Because they target different depths and mechanisms, combining both treatments may lead to more comprehensive improvement in suitable patients than either treatment alone.
Variations That Enhance Collagen Stimulation
Several microneedling techniques are used to enhance collagen production by modulating the biological signals involved in healing, without altering the fundamental mechanism.
RF Microneedling
RF microneedling adds controlled thermal energy to the microneedling process. In addition to mechanical micro-injury, radiofrequency energy causes thermal collagen contraction and stimulates deeper dermal remodelling.
This combination can enhance collagen production at greater depths compared to traditional microneedling, while still preserving the epidermis. It offers the potential for dermal tightening without the tissue removal involved in ablative procedures.
Microneedling with PRP
Microneedling with platelet-rich plasma (PRP) aims to enhance collagen stimulation by introducing growth factors directly into the skin. PRP contains concentrated platelets that release growth factors, which may support fibroblast activity and promote collagen renewal. While the core mechanism remains controlled injury and repair, PRP helps amplify the skin’s healing response when used alongside microneedling.
Why Subcision and Microneedling Are Commonly Combined
Subcision and microneedling are commonly combined because they address different aspects of acne scarring.
Subcision focuses on releasing and lifting scars structurally and stimulating collagen in the lower dermis. Microneedling, in contrast, improves overall dermal texture through collagen renewal.
In practice, Subcision is usually performed first to correct deep anchoring beneath the scar. Microneedling was introduced later to support broader collagen remodelling and smooth surface irregularities. Combining Subcision and microneedling may help address both the deep structural component and the quality of surrounding skin. This dual-modality approach is often preferred for creating more even and longer-lasting improvement.
Safety and Recovery Differences Related to Collagen Stimulation
Safety and recovery profiles in these treatments differ because the depth of injury influences how the skin heals. Subcision involves deeper dermal and subdermal injury, which commonly leads to bruising and swelling. Collagen forms gradually as deeper tissues remodel, leading to more noticeable recovery time but also longer-lasting structural improvement.
Microneedling creates controlled injury in the superficial to mid-dermis, with minimal disruption to the epidermis. This results in shorter downtime and lower risk of complications, but the collagen response is slower and more gradual. The depth of injury explains both the variation in healing time and the type of collagen remodelling achieved.
Quick Answers to Common Questions
How do Subcision and microneedling differ in how they stimulate collagen?
Subcision stimulates deeper, focal collagen formation, while microneedling stimulates diffuse collagen renewal. They work through different mechanisms.
Does collagen produced by Subcision and Microneedling treatments last?
Yes. Collagen produced by these treatments can be long-lasting, particularly after Subcision, although ageing and lifestyle factors still affect the skin over time.
Can microneedling replace Subcision?
No. Microneedling does not release the fibrous bands that cause tethered scars, so it cannot replace Subcision in those cases.
How long does collagen remodelling take?
Collagen remodelling typically continues for 3 to 6 months after treatment, depending on the procedure and individual skin response.