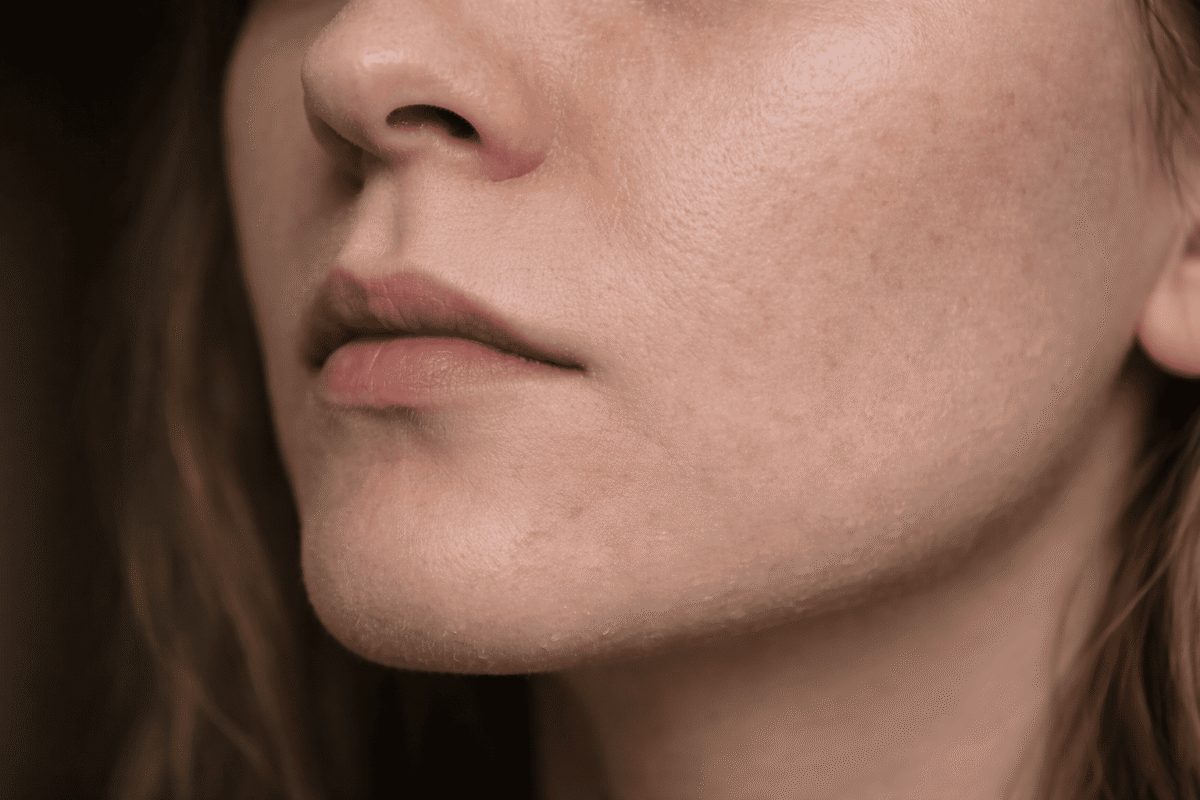Dull Skin: What is it, Causes, Treatments, and Prevention Tips
Dull skin may affect how your complexion looks and feels, often appearing tired or lacking radiance. Understanding its possible causes and knowing how to support your skin’s natural condition can help improve overall skin appearance over time.
In this article, we’ll explore the characteristics of dull skin, discuss common contributing factors, and share general care tips that may support a brighter, healthier-looking complexion.
What is Dull Skin?
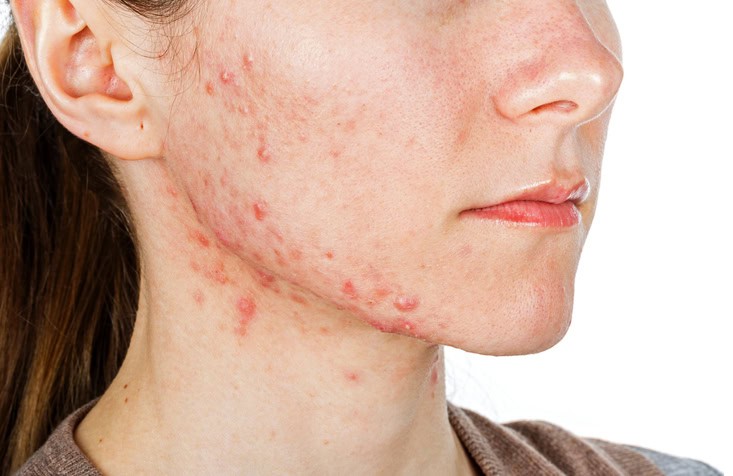
Dull skin is commonly described as skin that appears less smooth or less even in tone. It may feel dry or look flat, and can result from various internal or external factors.
Some characteristics often associated with dull-looking skin include:
- Rough texture: The skin may feel uneven or coarse to the touch.
- Less radiance: The skin may appear tired or less luminous than usual.
- Uneven tone: Areas of discolouration or patchiness may be more noticeable.
- Dryness or tightness: A lack of moisture can make the skin feel uncomfortable.
These features may affect how the skin looks in different lighting or under certain conditions.
Causes of Dull Skin
A variety of factors may influence how your skin looks and feels. Below are some common contributors that could affect skin texture and tone over time:
Environmental Factors
Elements such as sun exposure, pollution, and changing climates may impact the skin’s surface. For example, frequent sun exposure may contribute to changes in skin texture or tone, while environmental particles may settle on the skin, potentially affecting its clarity.
Lifestyle Habits
Daily habits such as poor sleep, limited hydration, or an unbalanced diet may influence how refreshed the skin appears. Stress and fatigue are also known to affect the skin’s overall condition.
Skincare Routine Mistakes
Skincare habits can also play a role. For instance, infrequent exfoliation may lead to a build-up of dead skin cells, while not using a moisturiser suited to your skin type might contribute to dryness. Choosing appropriate products and applying them consistently may support healthier-looking skin.
Treatments to Brighten Dull Skin
Managing dull skin often involves a combination of consistent skincare habits and, in some cases, professional support. Below is an overview of skincare products that may help support the skin’s appearance when used regularly.
1. At-Home Skincare Products

Incorporating suitable skincare products into your daily routine may support healthier-looking skin over time. Consider the following product types:
- Cleansers: A gentle, pH-balanced cleanser can help remove surface buildup without disrupting the skin’s moisture balance. Choose one that matches your skin type.
- Exfoliants: Exfoliation may assist in removing surface dead skin cells. Products that contain alpha or beta hydroxy acids (AHAs or BHAs) are commonly used to help improve skin texture.
- Moisturisers: Hydrating moisturisers help maintain skin comfort. Ingredients such as hyaluronic acid are often used in formulations designed to help attract and retain moisture.
- Serums: Some individuals choose brightening serums that contain ingredients like Vitamin C, which may support a more even-looking skin tone with regular use.
| Product Type | Active Ingredient | Benefits for Dull Skin |
|---|---|---|
| Gentle Cleansers | Hyaluronic Acid | Helps retain moisture, combating dryness and dullness. |
| Exfoliating Products | Glycolic Acid | Removes dead skin cells, promoting a smoother and brighter complexion. |
| Hydrating Moisturisers | Vitamin E | Provides antioxidant protection and hydrates the skin, enhancing radiance. |
| Brightening Serums | Vitamin C | Brightens skin tone and reduces pigmentation for a more even complexion. |
2. Professional Treatment
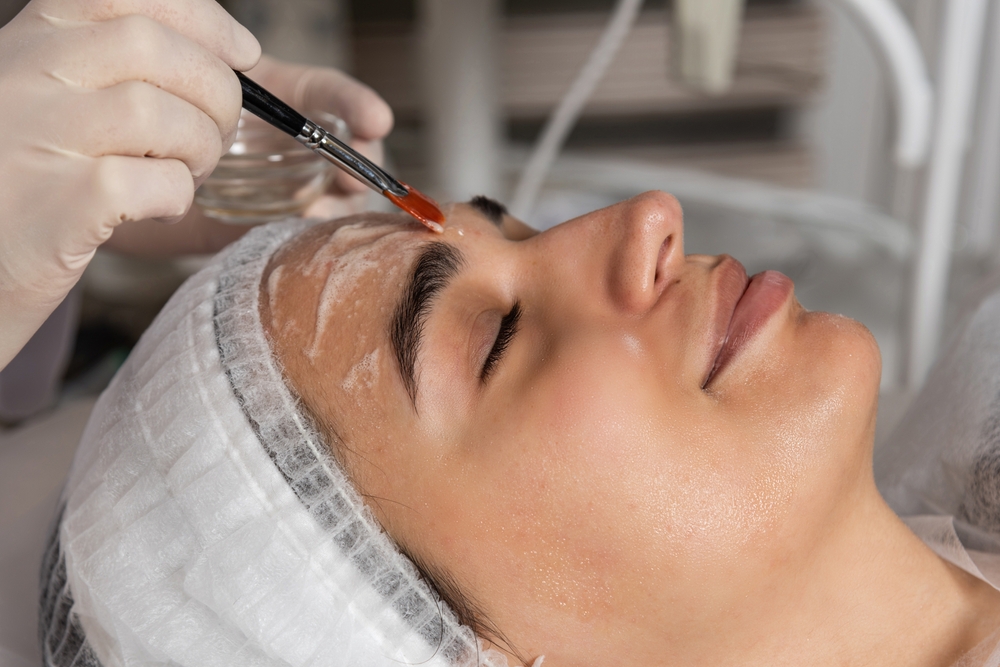
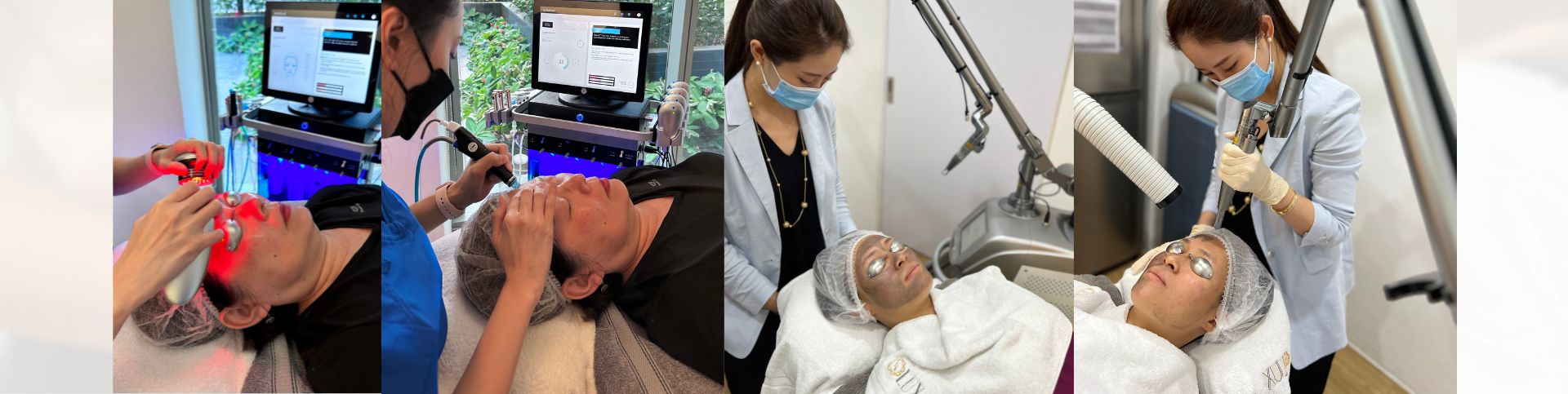
Some individuals may explore in-clinic options to support overall skin texture and clarity. These treatments are typically administered by trained practitioners and can be tailored to suit different skin concerns.
- Chemical Peels: This approach involves exfoliating the upper layers of the skin, which may support a smoother texture and more even appearance over time. Peels vary in strength and should be selected based on individual skin type and concerns.
- Laser Therapy: Light-based treatments may be used to support collagen stimulation and target concerns such as uneven skin tone. A qualified practitioner will determine the most suitable option depending on your skin’s condition.
- Microdermabrasion: This non-invasive treatment gently removes dead skin cells from the surface, supporting skin renewal and a smoother overall appearance.
Before undergoing any professional treatment, it’s important to consult a qualified practitioner who can assess your skin and recommend options suited to your individual needs.
Prevention Tips for Dull Skin
Simple lifestyle habits may help support the skin’s overall condition and reduce the likelihood of a dull or uneven appearance. Here are a few general tips to consider:
1. Keep Hydrated
Adequate hydration supports overall skin comfort and function.
- Drinking enough water throughout the day may help maintain moisture levels.
- A balanced diet with antioxidant-rich foods, such as berries and leafy greens, can also support skin health.
2. Use Sunscreen
Consistent sun protection may help protect the skin from UV-related changes.
- Choose a broad-spectrum sunscreen with an SPF suitable for your daily activities.
- Reapply as directed, especially during prolonged sun exposure.
3. Always Moisturise
Hydration through moisturisers helps to support the skin’s natural barrier.
- Select products suitable for your skin type: Look for moisturisers that contain hydrating ingredients like glycerin or hyaluronic acid.
4. Exfoliate Regularly
Exfoliation may help remove dead skin cells from the surface.
- Incorporate gentle exfoliation once or twice a week, depending on your skin’s needs.
- Avoid harsh scrubs that may cause irritation or damage to the skin barrier.
Vitamins and Supplements for Dull Skin
Some individuals consider vitamins or supplements as part of a broader approach to general well-being. While these options are not substitutes for a balanced diet or skincare routine, they may complement your efforts to support skin health.
- Vitamin C: Often associated with antioxidant properties, Vitamin C plays a role in supporting normal skin function. It is available through a variety of fruits, vegetables, and dietary supplements.
- Vitamin E: Known for its antioxidant role, Vitamin E contributes to the protection of cells from oxidative stress and may help maintain skin comfort.
- Vitamin D: Commonly obtained through sun exposure and food, Vitamin D supports overall health, including that of the skin.
- Collagen Supplements: Some people choose collagen products as part of their wellness routine. These may be used to complement other efforts, but evidence regarding their impact varies.
- Omega-3 Fatty Acids: Found in sources such as flaxseed oil and oily fish, Omega-3 fatty acids contribute to overall skin health by supporting lipid balance.
| Vitamin / Supplement | Benefits for Skin Health | Food Sources |
|---|---|---|
| Vitamin C | Supports collagen production and acts as an antioxidant. | Citrus fruits (oranges, lemons), strawberries, bell peppers, broccoli, kiwi. |
| Vitamin E | Acts as an antioxidant, protecting skin cells from damage. | Nuts (almonds, hazelnuts), seeds, spinach, broccoli, vegetable oils. |
| Vitamin D | May support skin barrier function and overall skin health. | Fatty fish (salmon, mackerel), egg yolks, fortified milk. |
| Collagen | Supports skin elasticity and hydration and may improve skin texture. | Bone broth, fish, chicken skin, collagen supplements. |
| Omega-3 Fatty Acids | Helps maintain the skin’s lipid barrier and may reduce inflammation. | Fatty fish (salmon, sardines), flaxseeds, chia seeds, walnuts. |
When to Seek Professional Help

If you’re concerned about persistent changes in your skin’s appearance, seeking advice from a qualified professional may offer further insights and options tailored to your needs. Here are some situations where professional input could be helpful:
Persistent Dullness
If your skin continues to appear lacklustre despite a consistent at-home routine, a professional consultation may help identify contributing factors and recommend suitable treatment options.
Changes in Skin Texture or Tone
Noticing increased roughness, uneven tone, or dry patches may suggest your skin requires a more tailored approach. A trained practitioner can assess your skin and offer guidance on next steps.
Acne or Blemishes
If blemishes or frequent breakouts accompany dullness, this may indicate that your current products aren’t well-suited to your skin type. A skincare professional may assist in refining your routine.
Signs of Irritation or Sensitivity
Increased sensitivity or irritation after using certain products may suggest your skin barrier has been affected. A practitioner can help identify possible irritants and recommend more suitable alternatives.
Lack of Improvement with Over-the-Counter Products
If non-prescription skincare products aren’t producing the results you’re aiming for, a professional can help explore other options, which may include clinic-based treatments or adjustments to your regimen.
Conclusion
Dull skin is a common concern that may influence how your skin looks and feels. Fortunately, it can often be supported by a consistent skincare routine that includes practices such as sun protection, regular exfoliation, and adequate hydration. A balanced diet and the appropriate use of skincare products may also help maintain the skin’s overall condition.
For individuals seeking further support, professional treatments may offer additional options. If dullness persists despite lifestyle adjustments, it may be helpful to speak with a qualified practitioner who can provide guidance tailored to your skin’s unique needs.