What Is the Difference Between Fractional CO2 Laser and Pico Laser for Acne Scars?
Fractional CO₂ and pico lasers are two types of energy-based devices used in managing acne-related skin texture changes. While both may support collagen activity and skin remodelling, they work through different mechanisms and are considered for different skin types and scar patterns.
Rather than one being superior to the other, the choice between them depends on factors such as scar depth, overall skin condition, tolerance for downtime, and individual response to treatment.
How Laser Treatments Help Acne-Related Scarring
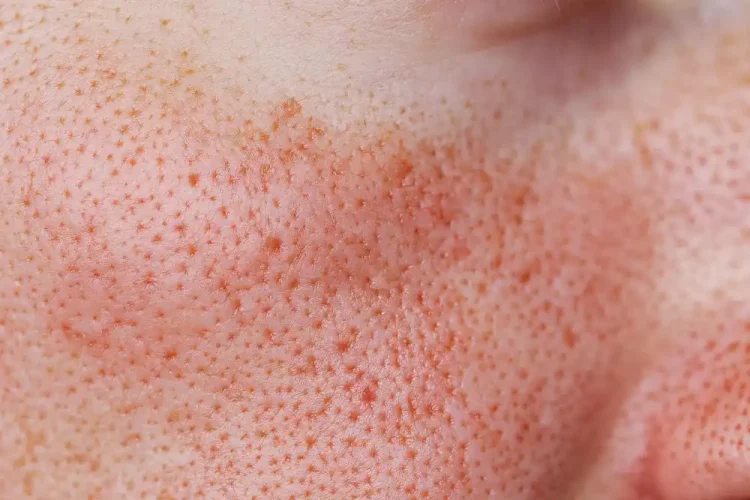
Acne scars can develop when inflammation interferes with the skin’s healing process. Two main factors often contribute to this:
- Collagen loss occurs when the skin produces insufficient collagen during healing, leading to depressed or uneven areas.
- Dermal structural damage occurs when inflammation alters the architecture of the deeper skin layers, resulting in permanent textural irregularities.
Laser treatments help address these concerns by using controlled energy to activate the body’s natural healing response. This process can support collagen activity in deeper layers or gently remove surface irregularities, depending on the type of laser used.
- Ablative lasers, like fractional CO₂, remove very small columns of skin to encourage tissue renewal and remodelling.
- Non-ablative lasers, such as pico lasers, keep the surface intact while using light-based energy to reach deeper layers of the skin.
These differences influence the recovery time and intensity of each option. Ablative lasers, such as fractional CO₂, may be considered when surface texture changes are more pronounced, whereas non-ablative lasers, such as picosecond lasers, are preferred when gentler approaches are preferred.
What Is Fractional CO₂ Laser for Acne Scars?
Fractional CO₂ laser is an ablative laser treatment commonly used for moderate to severe acne scarring. It is generally used when scarring affects both the surface and underlying dermal layers, where collagen loss and structural changes may be present. Due to its ablative nature, this approach is usually considered when less intensive options may not sufficiently address deeper texture concerns.
How Fractional CO₂ Laser Works
Fractional CO₂ laser works through ablative fractional resurfacing, a process that delivers laser energy in a grid-like pattern to the skin. The laser creates controlled microscopic columns of injury while leaving surrounding areas intact. These targeted micro-injuries activate the skin’s natural repair process, which can support collagen activity in both superficial and deeper skin layers over time.
As healing progresses, new collagen replaces damaged tissue, leading to gradual improvement in scar depth, skin texture, and overall smoothness.
Which Acne Scar Types Are Commonly Managed with Fractional CO₂ Laser
Fractional CO₂ laser is often considered for acne scars that involve both surface texture irregularities and deeper dermal changes. Scar patterns where this approach may be discussed include:
- Rolling scars, particularly when fibrous tethering is minimal or has been addressed
- Boxcar scars, especially shallow to moderate scars with defined edges
- Mixed atrophic scars, often as part of a broader treatment plan
For deeper rolling scars, fractional CO₂ laser can be used after subcision, once tethering beneath the skin has been released, to address surface texture changes.
Considerations When Using Fractional CO₂ Laser
One of the strengths of fractional CO₂ laser is its ability to support visible changes after fewer sessions compared to less intensive treatments. Collagen remodelling may continue for a period of time after treatment as part of the skin’s natural healing process. For this reason, it is often considered in cases of moderate to more established acne scarring.
Because it acts at both surface and deeper skin levels, fractional CO₂ laser is commonly used for deeper atrophic acne scars when performed by experienced practitioners and with appropriate patient selection.
Limitations and Risks of Fractional CO₂ Laser
Because it is an ablative treatment, it involves higher downtime, typically including redness, crusting, and peeling during the recovery period. Healing time varies depending on treatment intensity and individual skin response. There is also a higher risk of post-inflammatory hyperpigmentation (PIH), particularly in patients with darker skin types. This makes careful patient selection, conservative settings, and experienced technique essential.
Fractional CO₂ laser is also not ideal for ice-pick scars when used alone, as these narrow, deep scars often require targeted treatments such as chemical reconstruction rather than broad resurfacing.
What is a Pico (Picosecond) Laser for Acne Scars?
Pico, or picosecond, laser is a non-ablative laser technology used to improve acne scars by stimulating collagen without removing the skin surface. Unlike fractional CO₂ lasers, pico lasers target the dermis with minimal disruption to the skin surface, making them a consideration for certain scar types in which a less intensive approach is appropriate.
How Pico Laser Works
Pico laser delivers energy in ultra-short picosecond pulses, which are significantly shorter than those used in traditional lasers. These pulses create a photoacoustic effect, generating mechanical shock waves rather than relying primarily on thermal effects. This effect supports dermal remodelling while keeping the skin surface intact. Because a pico laser is non-ablative, it does not remove skin layers. Instead, it produces controlled dermal stimulation that gradually improves skin texture and scar appearance over multiple sessions.
This mechanism explains why pico laser typically involves minimal downtime but also more gradual results.
What Types of Acne Scars Respond to Pico Laser
Pico laser is often considered for patients with:
- Mild or shallow atrophic scars
- Uneven skin texture or surface irregularities
- Scars with overlapping pigmentation, such as post-inflammatory hyperpigmentation
For deeper scars, pico laser may be used in combination with other techniques to support ongoing scar management or refine surface texture.
Considerations for Pico Laser
Pico laser is associated with shorter recovery periods compared with more intensive resurfacing treatments. Some individuals may experience mild redness, and many can resume daily activities within a short period.
Pico laser is often considered for darker skin types, as it delivers energy with less reliance on heat when appropriate settings are used. As a result, the risk of post-inflammatory hyperpigmentation (PIH) is generally lower when appropriate settings are used.
These features are often considered when discussing pico laser with patients who prioritise shorter recovery periods and gradual treatment response.
Limitations of Pico Laser
As a non‑ablative treatment, pico laser produces changes that tend to develop gradually across sessions. Treatment plans often involve multiple sessions, depending on individual response and treatment goals.
Pico laser may be less suited for deep acne scars, particularly those associated with marked collagen loss or dermal tethering. In such cases, other treatment approaches or combination strategies are often required.
Fractional CO₂ and Pico Laser Key Differences
This table summarises the differences between fractional CO₂ laser and pico laser for acne scar treatment. This comparison highlights why these lasers are not interchangeable, but instead serve different roles depending on scar type and patient factors.
| Comparison Dimension | Fractional CO₂ Laser | Pico (Picosecond) Laser |
|---|---|---|
| Mechanism | Ablative fractional resurfacing | Non-ablative photoacoustic stimulation |
| Depth of action | Surface and deeper dermal layers | Primarily dermal stimulation |
| Scar types commonly considered | Rolling scars, boxcar scars, mixed atrophic scars | Mild scars, texture irregularities, pigmentation-associated scars |
| Number of sessions needed | Involves fewer sessions in some treatment plans | Often involves multiple sessions |
| Downtime and recovery | Moderate to higher downtime | Minimal downtime |
| Skin type considerations | Requires careful settings and aftercare in darker or melanin-rich skin types | Often considered for darker skin types when conservative parameters are used |
| Typical cost positioning | Higher per-session cost due to treatment intensity | Lower per-session cost, with multiple sessions often planned |
Downtime and Recovery
Downtime is a key practical difference between fractional CO₂ and pico lasers and often plays a significant role in treatment planning.
Fractional CO2 Laser
Fractional CO₂ laser typically involves moderate downtime. Common effects may include redness, swelling, crusting, and peeling. Healing usually takes place in stages:
- Initial inflammation and oozing
- Formation of micro-crusts
- Gradual skin renewal and fading of redness
Recovery varies depending on treatment intensity and individual skin response, but most patients experience downtime lasting several days.
Pico Laser
Pico laser treatment can cause temporary redness or swelling, and many individuals resume normal activities soon after. Because the skin surface is left intact, recovery is generally shorter than with ablative laser procedures. This shorter downtime may be more suitable for individuals who prefer gradual improvements or have limited time for recovery.
Safety and Skin Type Considerations
Skin type plays an important role in determining how the skin responds to laser treatments, particularly regarding the risk of post-inflammatory hyperpigmentation (PIH).
Fitzpatrick Skin Types I–III
Individuals with lighter skin types may tolerate a broader range of laser settings, including ablative treatments like fractional CO₂ laser, when appropriately selected and performed. The risk of pigmentary changes is generally lower in this group when post-treatment care is followed properly.
Fitzpatrick Skin Types IV–VI
For individuals with darker or melanin-rich skin, there is a higher likelihood of PIH following ablative laser procedures. In such cases, treatments such as picosecond lasers may be considered, as they do not remove skin layers and are associated with a lower risk of surface disruption when conservative parameters are used.
Importance of a Clinical Experience
Regardless of skin type, provider expertise is essential. Appropriate laser choice, customised treatment settings, and thorough post-procedure care all contribute to both treatment safety and effectiveness. Practitioners experienced in treating a range of skin types are better positioned to minimise risks and tailor the treatment plan to individual needs.
Can Fractional CO₂ and Pico Lasers Be Combined?
Combination treatment is often considered, as fractional CO₂ and pico lasers target different layers of acne scarring.
A typical sequence may include:
- Fractional CO₂ laser first, to target deeper structural changes and support collagen remodelling
- Pico laser later, to refine texture and address residual pigmentation
While this approach may involve a higher upfront cost, it may offer a more layered strategy for scar management when tailored to individual concerns.
FAQs
Is fractional CO₂ laser more suitable than pico laser for acne scars?
No. Fractional CO₂ laser therapy is often considered for deeper acne scars, whereas picosecond laser therapy is more appropriate for mild scarring or when pigmentation is also a concern. The appropriate option depends on the individual’s skin condition, scar type, and treatment goals.
Can pico laser treat deep acne scars?
Pico laser’s effect on deeper acne scars is limited. It is often used as part of a broader treatment plan rather than as a standalone approach for more pronounced scarring.
Can pico laser replace fractional CO₂ laser entirely?
Pico laser is not typically used as a full replacement for fractional CO₂ laser in treating moderate to deep acne scars, but may be considered in combination or for maintenance.