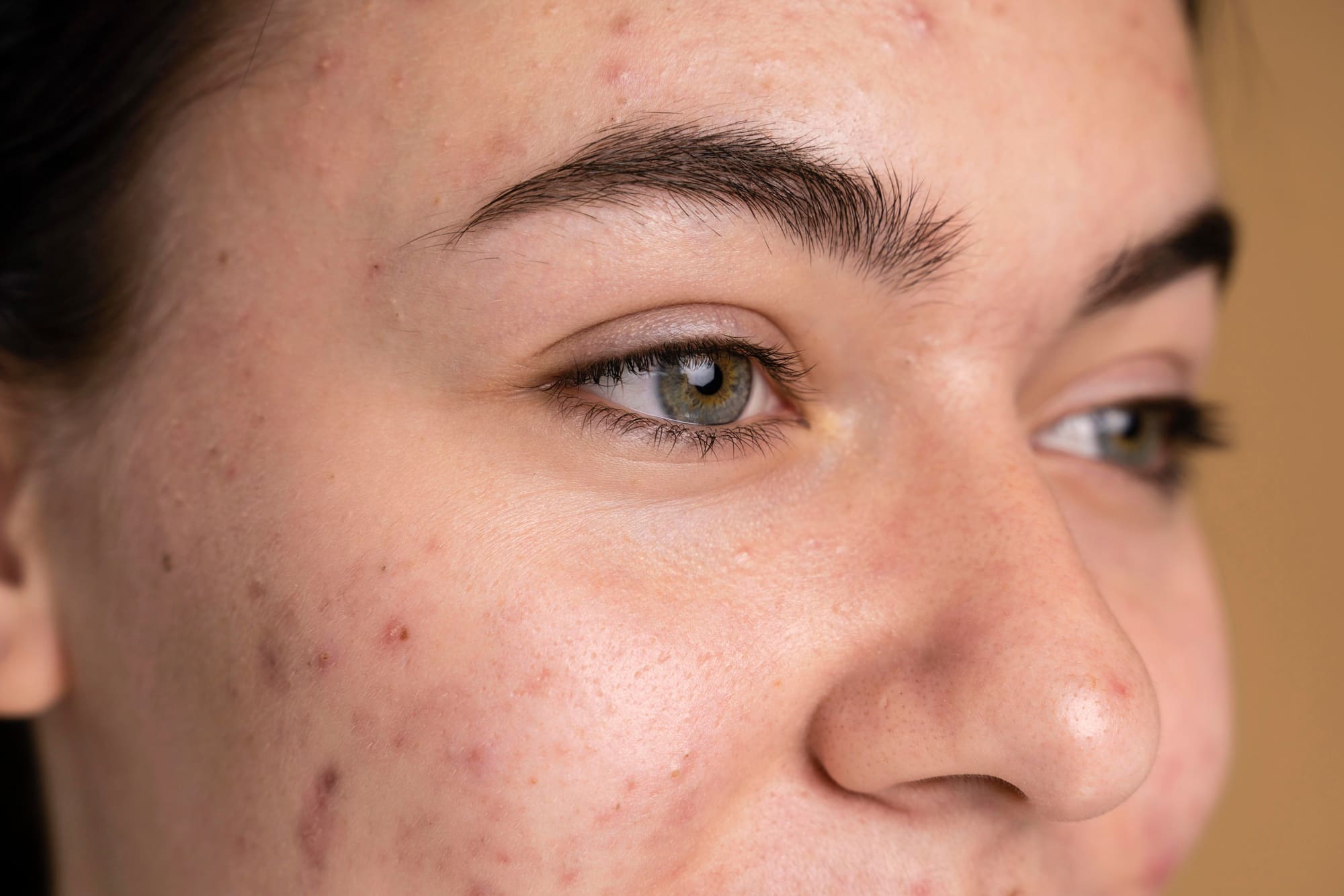
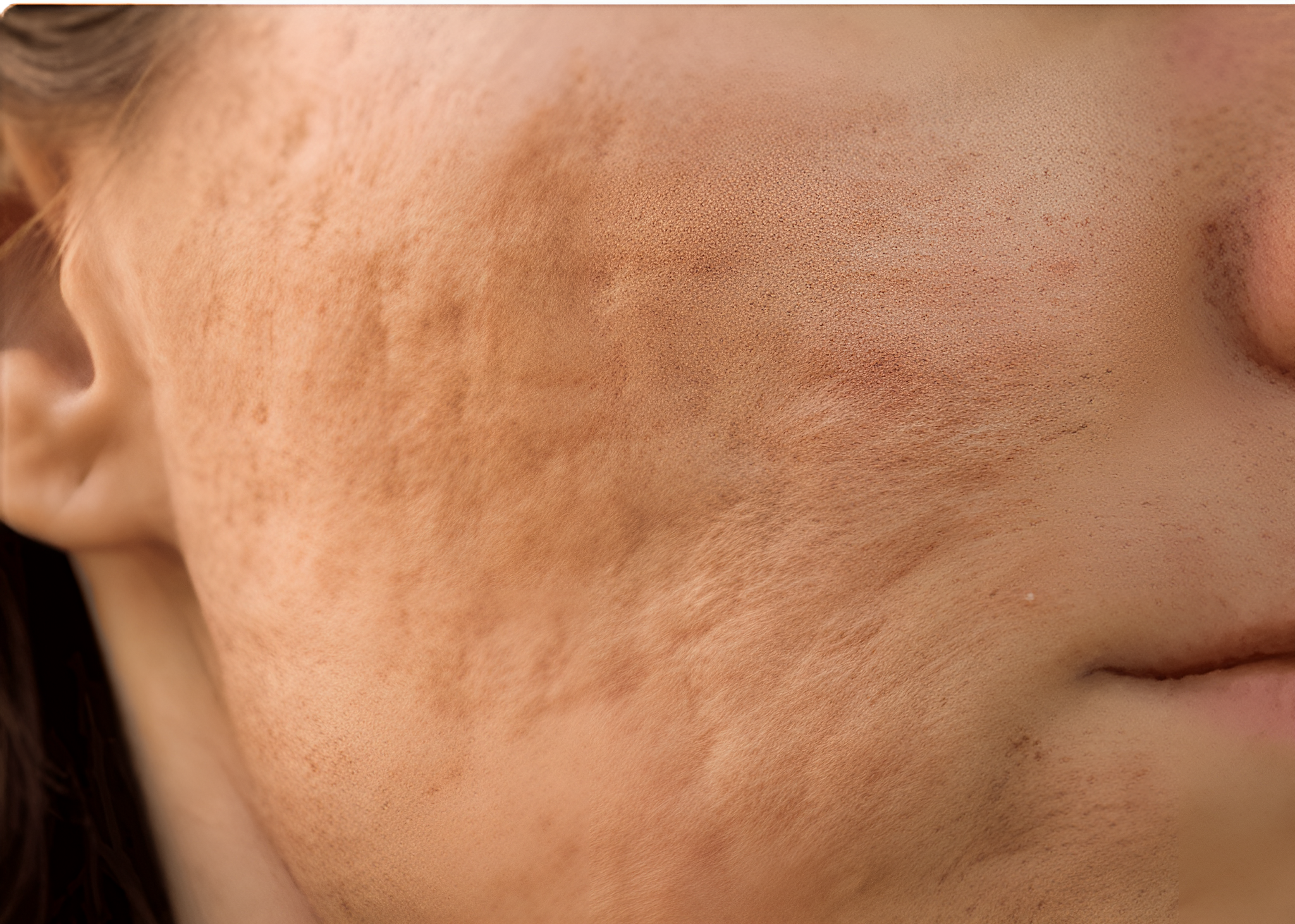
Many individuals experience both post-acne pigmentation and acne scarring, often from the same breakout. While these concerns may occur together, they arise from separate biological processes. Because the underlying causes differ, not all treatments are suitable for both concerns. Some methods may improve both tone and texture, whereas others are more targeted and should be combined for optimal results.
This article outlines how dual-action treatments are selected, when they may be appropriate, and why addressing pigmentation and scarring separately can be safer and more effective, particularly in skin types prone to post-inflammatory hyperpigmentation (PIH). It also highlights how treatment plans are typically structured in clinical practice across Singapore.
Understanding Pigmentation and Acne Scars
Pigmentation after acne, or post-inflammatory hyperpigmentation (PIH), happens when the skin produces excess melanin in response to inflammation. Acne scars, by contrast, result from collagen loss and structural changes in the skin during the healing process.
Overlap occurs because both problems can arise from the same inflammatory acne episode, particularly when healing is prolonged or disrupted. However, it is important to clarify that treating pigmentation does not automatically correct scars, and improving scars does not necessarily resolve pigmentation. Each concern must be evaluated independently, even when they coexist.
What Makes a Treatment Dual-Action?
A treatment is considered dual-action when its biological effects can influence both skin colour and skin texture, even if one effect is secondary. These effects typically arise from broader mechanisms rather than from direct targeting of both problems.
Mechanisms that may influence both pigmentation and scarring include:
- Mild epidermal turnover, which can support pigment normalisation
- Dermal collagen stimulation, which improves scar structure and may indirectly improve skin tone uniformity
- Reduction of chronic inflammation, which benefits both melanin activity and collagen repair
Dual-action effects are often supportive rather than definitive, which is why expectations must be adjusted and outcomes assessed separately for pigment and scars.
Categories of Treatments With Overlapping Benefits
Rather than viewing the treatment as an all-in-one solution, they are often grouped by primary role and secondary effect.
Collagen-Stimulating Treatments With Secondary Pigment Benefits
These treatments are primarily selected to improve skin structure and scar texture by stimulating collagen production in the dermis. As collagen quality improves and skin turnover normalises, pigmentation may improve gradually as a secondary effect, particularly when inflammation is reduced.
Commonly used treatments in this category include Microneedling, RF microneedling and Subcision (when combined with adjunctive treatments).
Typical clinical role:
- Scar-focused, with pigment-supportive benefits
- Often combined with pigment-specific treatments rather than used alone for PIH
Doctors generally do not rely on these treatments as standalone solutions for significant pigmentation, but they may contribute to overall tone improvement as part of a structured plan.
Pigment-Targeting Treatments With Mild Texture Effects
These treatments are primarily chosen to address uneven skin colour, including post-inflammatory hyperpigmentation. Any improvement in texture or scarring is usually subtle and limited to shallow irregularities.
Examples in this category include:
- Picosecond (pico) lasers
- Q-switched pigment lasers
- Superficial chemical peels
Typical clinical role:
- Pigment-focused, with minor texture refinement
- More appropriate when pigmentation is the dominant concern and scarring is mild
These treatments primarily treat pigmentation, and their effect on deeper scar texture is limited.
Skin Resurfacing Treatments
Treatments, such as superficial chemical peels and non-ablative fractional lasers, promote surface-level skin renewal, which may even out pigmentation and gently improve texture over time. However, they do not address deeper acne scars.
Typical clinical role:
- Supportive or maintenance treatment.
- Often used between more targeted pigment or scar procedures.
These approaches are usually supportive rather than corrective for acne scars, helping clinicians set proper expectations for outcomes.
Treatments Used as Part of Combination Plans
Certain treatments may help with both pigmentation and scarring, but they often work best when combined with other procedures rather than used on their own.
Examples include:
- Subcision with pico laser
- RF microneedling and pigment-targeting lasers
- Non-ablative fractional lasers combined with topical maintenance
Typical clinical role:
- Addressing both colour and structure through sequencing
- Allowing each concern to be treated using its most appropriate mechanism
This approach prioritises safety, careful control of post-inflammatory hyperpigmentation (PIH) risk, and gradual improvement over time.
When Dual-Action Treatments May Be Appropriate
Dual-action treatments are generally suited for mild to moderate acne scars with residual post-inflammatory hyperpigmentation, especially when scars are shallow and not deeply tethered. They may also be used for early or surface-level atrophic scars, where uneven skin tone contributes more to the appearance than deeper structural damage.
This type of strategy may appeal to patients who prefer shorter downtime and gradual improvement.
In cases of more severe scarring or persistent pigmentation, separate or staged plans are often more suitable. Trying to treat both concerns aggressively in the same session can increase the risk of irritation or other complications without leading to better overall results.
When Staged Treatment May Be More Suitable
In some cases, treating pigmentation and acne scars together is not ideal. The decision depends on how the scars behave and on the skin’s reactivity.
Separate or staged plans are often considered when:
- Scars are more severe or deeply tethered
- Pigmentation is persistent or prone to recurrence
- The skin has a history of post-inflammatory hyperpigmentation (PIH)
- Inflammation needs to be carefully controlled over time
When scars are mild and relatively shallow, a combined strategy may be reasonable. This is especially true if uneven tone contributes more to the appearance than structural depth.
However, attempting to address both concerns aggressively in a single session may increase irritation, prolong recovery, or trigger further pigmentation. Addressing each issue in stages often allows for better control of skin response.
Skin Type Considerations
In Singapore, many patients have Fitzpatrick skin types III–V, which are more prone to post-inflammatory hyperpigmentation. In addition, heat and year-round UV exposure act as constant triggers for melanin production, even outside direct sun exposure.
To reduce risks, treatment plans are often tailored by:
- Using conservative energy or depth settings
- Staging pigmentation and scar treatments rather than combining them in a single session
- Emphasising ongoing maintenance, skincare routines, and consistent sun protection
Treatment success depends not just on the device used, but also on clinical judgement, careful planning, and appropriate aftercare. Familiarity with Asian skin types is important for ensuring treatment safety and achieving consistent outcomes.
Managing Expectations for Combined Pigment and Scar Treatments
Pigmentation and acne scars do not improve at the same pace. Pigment often fades earlier during treatment, while changes in scar texture usually take longer to see. Scar improvement depends on collagen remodelling beneath the skin, and that process develops gradually.
For many patients, moderate improvement in both pigmentation and scarring is a realistic goal. Complete resolution is uncommon, particularly in long-standing or deeper scars.
Ongoing maintenance is often needed, particularly for pigmentation. Recurrence may occur due to:
- Sun exposure
- Hormonal influences
- Inflammation or skin irritation
Recognising these differences helps guide treatment planning and reduces the need for overly aggressive procedures.
FAQs
Why do some treatments improve pigmentation more than scarring?
Because they primarily target melanin in the skin rather than the deeper layers, where collagen remodelling is needed for scar improvement.
Is it better to treat pigmentation or scars first?
It depends on the skin’s condition. Doctors typically consider factors such as pigmentation risk, skin sensitivity, and scar depth before making a decision.
Are dual-action treatments safer for Asian skin?
They can be, especially when used with conservative settings and realistic expectations.
Why are staged treatment plans often recommended?
Separating pigment and scar treatments can help reduce the risk of irritation and improve the safety and predictability of results.