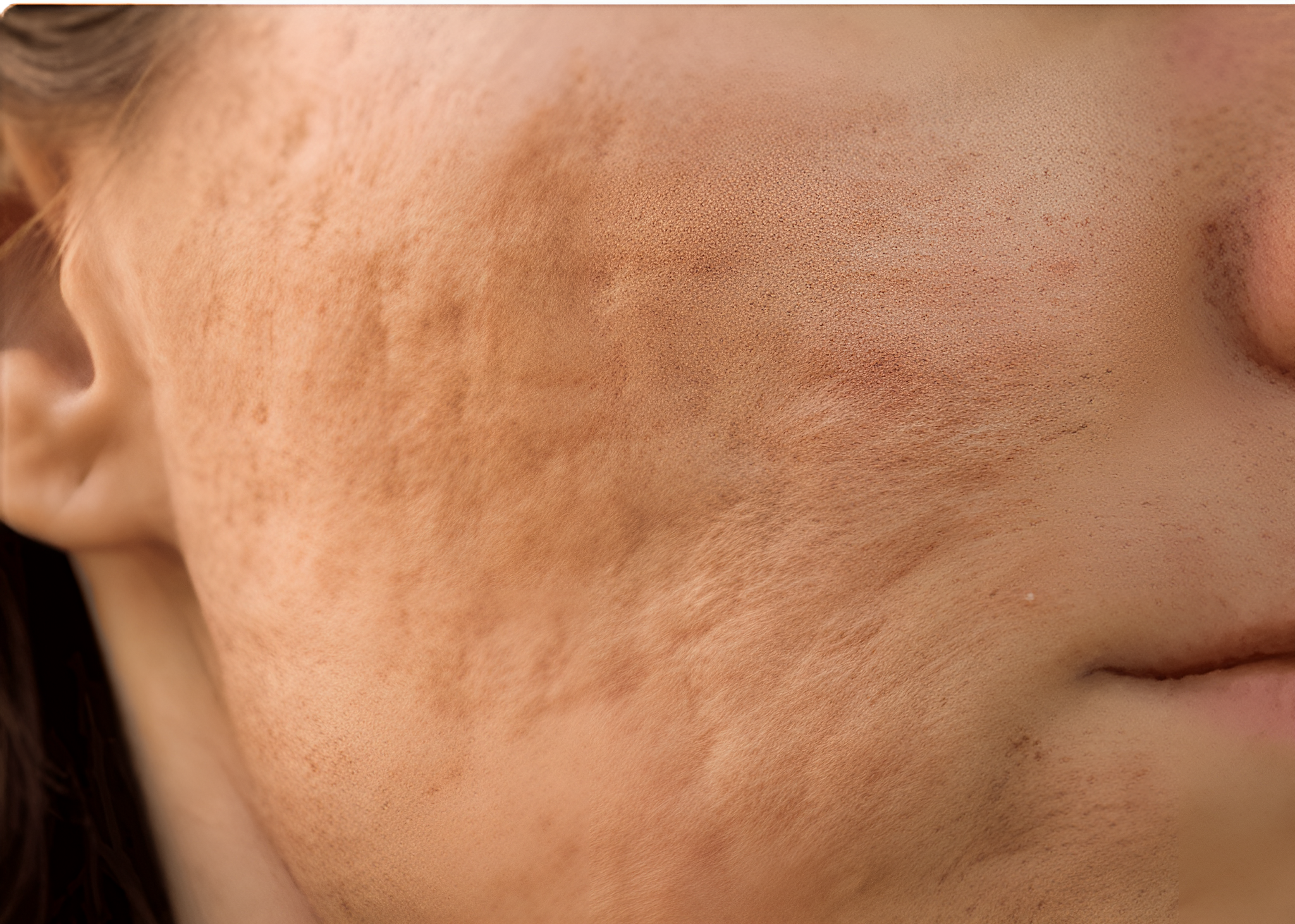
Concerns about risks and side effects are common before undergoing acne scar treatment. Most procedures used to improve acne scars work by creating controlled injury in the skin to stimulate collagen remodelling. Consequently, temporary changes during healing are expected.
All medical procedures carry some degree of risk. However, acne scar treatments are generally considered low risk when they are properly assessed, planned, and performed in an appropriate clinical setting. The likelihood and type of side effects depend on several factors, including treatment type, intensity, skin type, and individual healing response.
This article explains the difference between normal side effects and true complications, outlines common and less common risks, and clarifies how doctors work to minimise them. Understanding these factors helps patients approach treatment with realistic expectations and informed decision-making.
What Doctors Mean by Side Effects and Complications
Before discussing risks, it helps to clarify the terms doctors use during consultation. Understanding the difference between side effects and complications can reduce unnecessary anxiety and set realistic expectations.
Side effects are expected and temporary responses to treatment. They occur as part of the normal healing process when the skin reacts to controlled injury. Examples include redness, swelling, peeling, or mild bruising. These changes typically improve on their own and do not lead to long-term problems.
Complications, in contrast, are unintended or prolonged reactions. They fall outside the usual healing pattern and may require medical review, closer monitoring, or additional treatment.
Recognising this distinction helps patients understand what is normal during recovery and when further evaluation may be needed.
Common Side Effects After Acne Scar Procedures
After acne scar treatment, certain changes are expected as part of the skin’s normal healing response. The type and intensity of these effects depend on the procedure performed and individual skin sensitivity. In most cases, they are temporary and improve as the skin recovers.
- Swelling: Mild to moderate swelling may occur, particularly after subcision or injectable treatments. This usually settles within a few days as inflammation reduces.
- Tenderness or Soreness: The treated area may feel sensitive or slightly painful for a short period, depending on the intensity of treatment.
- Peeling or Flaking: Superficial peeling may occur after chemical peels or laser procedures. This reflects skin renewal and typically resolves as new skin forms.
- Temporary Darkening of Pigment: Some patients notice temporary darkening before lightening occurs. This can happen during the healing process, particularly in pigment-prone skin.
- Mild Bruising: Bruising may occur after subcision or injection due to minor disruption of blood vessels. It generally fades over one to two weeks.
These responses are usually self-limiting and improve with appropriate aftercare. Monitoring progress and following post-treatment instructions support predictable recovery.
Less Common but Important Risks to Be Aware Of
Most patients experience temporary and expected side effects. However, less common reactions can occur and may require closer monitoring or medical review. The likelihood of these risks depends on treatment type, skin characteristics, and aftercare.
Post-Inflammatory Hyperpigmentation (PIH)
Post-inflammatory hyperpigmentation (PIH) is one of the more frequently discussed risks in acne scar treatment, particularly in darker skin types.
The risk is higher in:
- Fitzpatrick skin types III–VI
- Treatments performed at high intensity
- Sessions spaced too closely together
PIH is often temporary, but it may take several weeks to months to fade, depending on individual skin response.
Infection
Infection is uncommon when procedures are performed using proper technique and when aftercare instructions are followed.
The risk increases with:
- Inadequate wound care
- Picking at treated areas
- Contamination during healing
Early recognition and treatment are important to reduce the likelihood of longer-term complications.
Prolonged Redness or Inflammation
Some patients may experience redness that lasts longer than expected. This is more commonly associated with:
- Ablative laser treatments
- Deep chemical peels
In most cases, redness gradually improves, although monitoring may be needed if it persists.
Scarring or Texture Changes
Worsening scarring or unintended texture changes are uncommon. When they occur, they are often linked to:
- Excessive treatment depth
- Delayed or impaired healing
- Underlying skin conditions
Careful assessment and appropriate treatment settings help reduce this risk.
Pigment Lightening (Hypopigmentation)
Hypopigmentation, or lightening of the skin, is rare but may occur after aggressive resurfacing procedures. It can be more challenging to manage than post-inflammatory darkening, which is why conservative treatment planning is important.
Risks by Treatment Category
The type of acne scar procedure influences the recovery pattern and potential risks. While most side effects are temporary, the intensity and depth of treatment affect how the skin responds.
Microneedling / RF Microneedling
Microneedling procedures create controlled micro-injuries to stimulate collagen production.
Common side effects include:
- Temporary redness
- Mild swelling
- Short-term skin sensitivity
When performed using conservative settings and appropriate spacing, the risk of post-inflammatory hyperpigmentation (PIH) is generally low. Risk may increase with aggressive parameters or inadequate aftercare.
Laser Treatments (Non-Ablative vs Ablative)
Laser procedures vary in depth and intensity, which influences recovery and risk.
Non-ablative lasers
These treatments do not remove the outer layer of skin.
- Typically involves shorter downtime
- Lower risk of prolonged redness
- PIH risk depends on skin type and the settings used
Ablative lasers
These treatments remove portions of the skin surface to resurface deeper layers.
- Longer recovery period
- Higher risk of post-inflammatory hyperpigmentation, particularly in pigment-prone skin
- Greater likelihood of prolonged redness
Strict aftercare and sun protection are important after ablative procedures.
Subcision
Subcision releases fibrous bands beneath tethered scars.
Common side effects include:
- Bruising
- Swelling
- Temporary firmness in the treated area
Less common risks include uneven healing or persistent nodules, which may require review.
Chemical Peels
Chemical peels remove controlled layers of skin to improve texture and pigmentation.
Possible side effects include:
- Temporary irritation
- Peeling or flaking
- Pigment changes if the peel is too strong for the skin type
The risk of PIH increases without proper sun protection or when stronger formulations are used in pigment-prone individuals.
Dermal Fillers
Dermal fillers are used to support depressed scars by restoring volume beneath the skin.
Common side effects include:
- Swelling
- Bruising at injection sites
Rare but serious vascular complications can occur if filler enters a blood vessel. This risk is reduced when injections are performed by appropriately trained medical professionals.
Who Is at Higher Risk of Side Effects
While most acne scar procedures are considered low risk when properly planned, certain individuals are at higher risk of side effects.
Risk tends to be higher in patients with the following characteristics:
- Fitzpatrick skin types III–VI, as darker skin tones are more prone to post-inflammatory hyperpigmentation (PIH), especially after higher-intensity treatments
- A personal history of PIH following previous procedures
- Active acne or ongoing inflammation, which can make the skin more reactive during recovery
- A compromised skin barrier, often due to over-exfoliation, harsh skincare, or recent procedures
- Inconsistent sun protection habits, particularly in the weeks after treatment
These factors do not automatically rule out treatment, but they may require a more cautious approach. Identifying them early allows doctors to adjust the treatment plan appropriately and reduce unnecessary risk.
How Doctors Reduce Risks Before and After Treatment
Risk reduction starts with careful assessment. Doctors evaluate scar type, skin tone, pigmentation risk, and healing history before recommending a procedure.
During treatment, conservative energy or depth settings are used where appropriate, especially in pigment-prone skin. Sessions are spaced adequately to allow proper healing and reduce inflammation. In some cases, pre-treatment skincare is advised to stabilise the skin. Clear aftercare instructions and scheduled follow-up reviews help monitor recovery and address concerns early.
Careful planning, appropriate spacing, and good aftercare work together to minimise complications.
Normal Healing vs When to Seek Medical Review
After acne scar procedures, certain responses are expected as part of the healing process.
Common and usually temporary responses include:
- Redness that gradually improves
- Mild to moderate swelling
- Peeling or flaking
- Temporary pigment darkening
- Mild bruising, particularly after subcision or injections
These responses typically stabilise over days to weeks, depending on treatment depth.
Medical review is recommended if:
- Pain or redness progressively worsens
- Swelling becomes severe or asymmetrical
- Signs of infection appear, such as pus, fever, or spreading warmth
- Pigment changes persist or worsen unexpectedly
- Healing does not progress within the expected timeframe
Early evaluation allows appropriate management and reduces the likelihood of prolonged complications.
Can Risks Be Eliminated Completely?
No procedure is entirely risk-free. Acne scar treatments involve controlled injury to stimulate collagen remodelling, and any intervention carries some degree of variability in healing response.
However, risks can be significantly reduced through:
- Individualised treatment planning
- Appropriate patient selection
- Conservative, staged approaches
- Careful post-treatment care
- Consistent sun protection
Both clinical judgement and patient adherence contribute to safe outcomes.
FAQ
Is post-inflammatory hyperpigmentation permanent?
In many cases, PIH is temporary and gradually fades over weeks to months. Duration varies based on skin type, inflammation level, and sun exposure.
Are laser treatments riskier than microneedling?
Risk depends more on treatment depth, intensity, and skin type than on the device category alone. Ablative procedures generally involve longer recovery and a higher risk of pigment changes compared to non-ablative treatments.
Can side effects be prevented completely?
They cannot be completely prevented, but proper assessment, conservative settings, and good aftercare significantly reduce risk.
What should I do if my skin reacts badly?
Seek medical review promptly if symptoms worsen, signs of infection develop, or healing does not progress as expected.
How do doctors decide if a treatment is safe for me?
Doctors assess scar type, skin characteristics, pigmentation risk, medical history, and lifestyle factors before recommending a treatment plan.