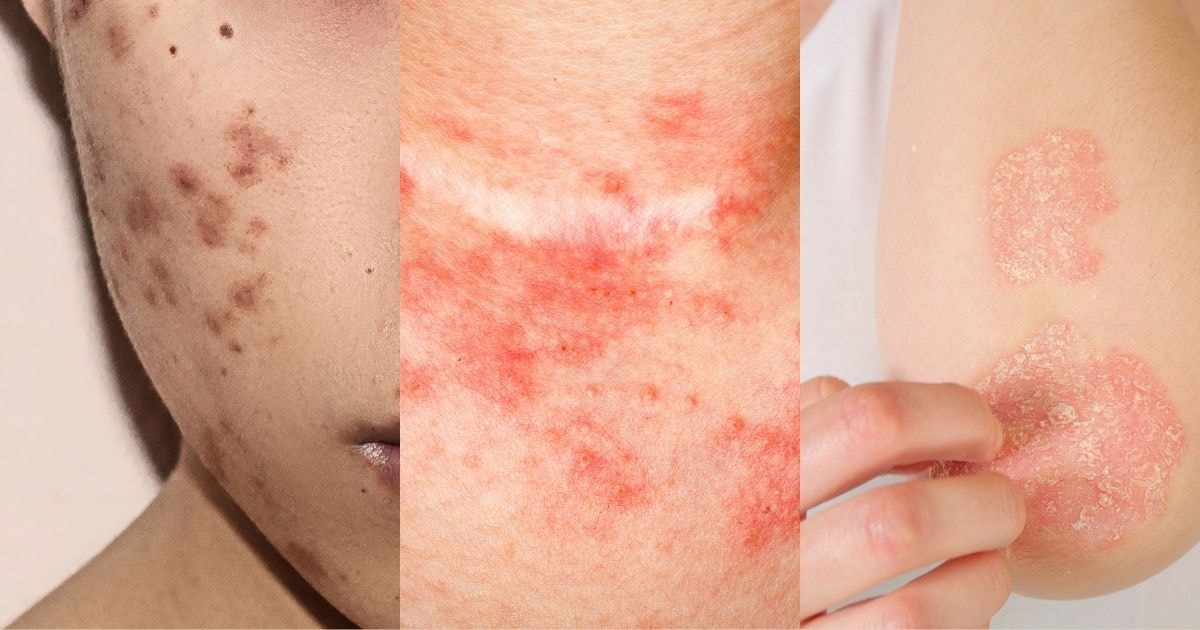
Post-inflammatory hyperpigmentation (PIH) is a common skin condition where dark spots or patches appear after the skin heals from an inflammation or injury.
This guide outlines the causes, symptoms, treatment options, and prevention strategies for post-inflammatory hyperpigmentation. We’ll also discuss situations where it may be helpful to consult a dermatologist or aesthetic practitioner.
What is Post-Inflammatory Hyperpigmentation?
Post-inflammatory hyperpigmentation (PIH) occurs when the skin produces excess melanin after an inflammatory event, such as acne, eczema or a cosmetic procedure (e.g., chemical peel or laser treatment).
The condition typically occurs in individuals with darker skin types (Fitzpatrick IV-VI) as their higher melanin levels make them more vulnerable to changes in pigmentation. The pigmentation can vary in hue, ranging from light brown to black and may even manifest as grey or blue in cases of deeper pigmentation.
How Does PIH Develop?
PIH develops when melanin production increases in response to inflammation or injury. The melanocytes in the skin, which produce melanin, become overactive during the skin’s healing process, leading to excessive melanin deposition in the epidermis or dermis. Epidermal PIH (affecting the outer skin layer) often responds differently to management compared to dermal PIH (deeper pigmentation), which may take longer to improve.
Causes of Post-Inflammatory Hyperpigmentation
Different triggers or events can contribute to the development of PIH. These triggers cause overproduction of melanin – the pigment responsible for skin colour. Melanin accumulates in the affected area, leaving behind dark spots or patches. Below are the most common causes of PIH:
1. Acne Vulgaris
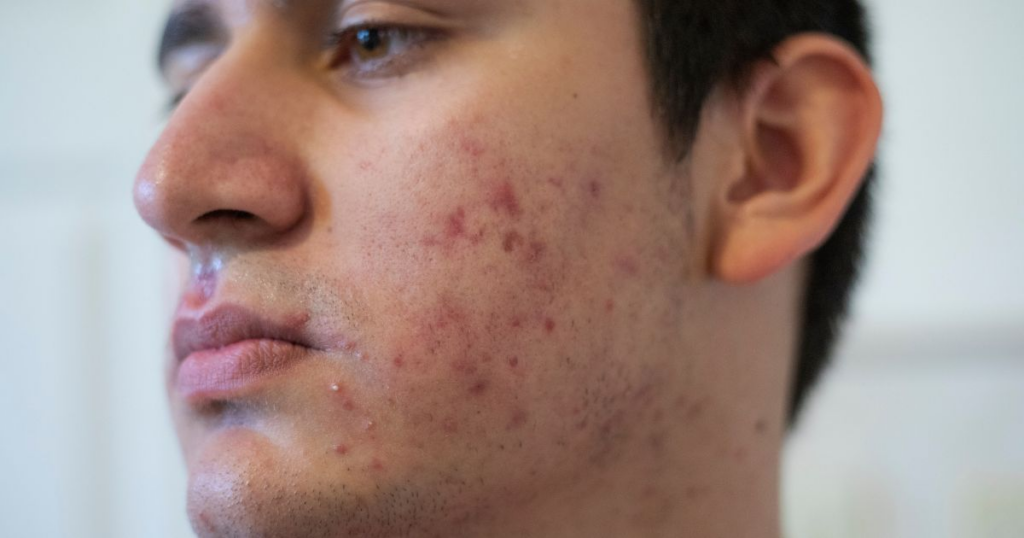
Inflammatory acne, particularly in forms like cysts or nodules, is one of the main causes of PIH. Prolonged inflammation from active acne lesions prompts melanocytes – cells responsible for pigment production – to generate excess melanin in the skin. This results in acne marks and PIH, often appearing as dark brown or purple spots.
Individuals with darker skin types may experience persistent facial post-inflammatory hyperpigmentation after acne vulgaris heals.
2. Eczema and Atopic Dermatitis
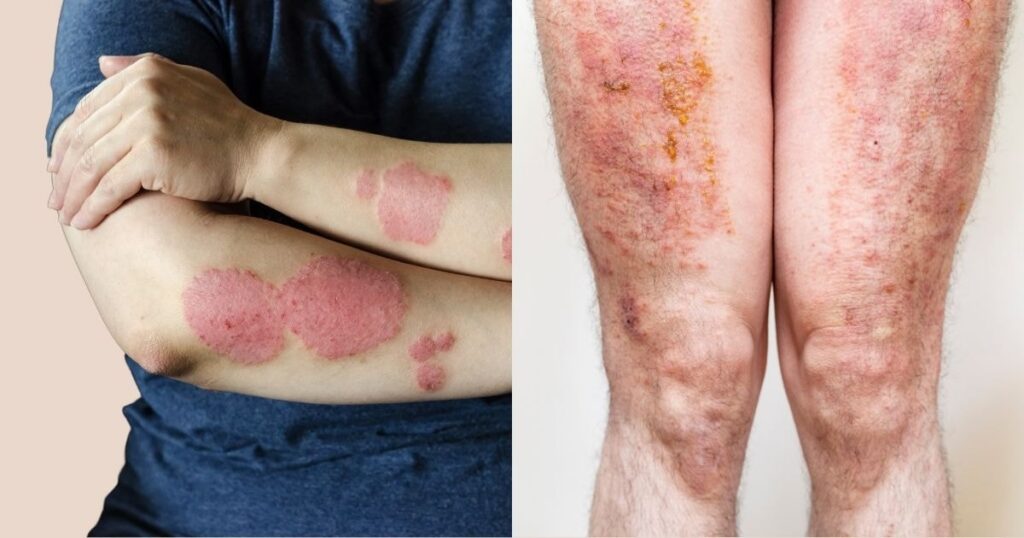
Chronic skin conditions like eczema and atopic dermatitis often cause frequent skin irritation, leading to intense scratching or rubbing. This mechanical trauma worsens inflammation, causing the skin to produce more melanin in the affected areas. Repeated flare-ups of eczema may also worsen the discolouration.
3. Skin Injuries or Trauma
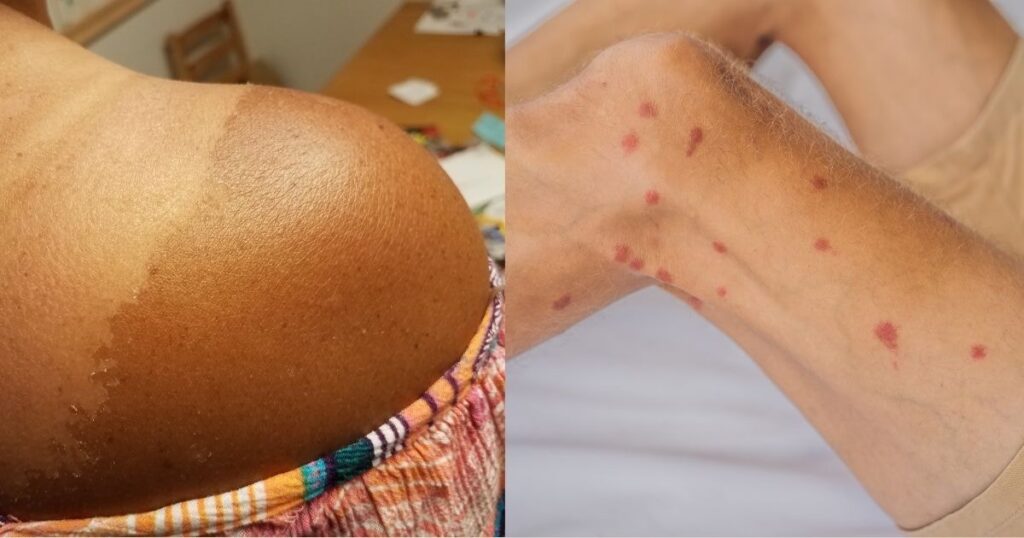
Physical trauma, such as picking acne and scratching other lesions, cuts, burns, or even insect bites, can initiate an inflammatory response. This response results in excess melanin during the healing process. These injuries, particularly in areas exposed to UV light, can lead to persistent PIH.
4. Allergic Reactions

Allergic reactions that result in skin inflammation, such as reactions to certain skincare ingredients or environmental allergens, can also lead to PIH.
5. Some Cosmetic Procedures (Laser Treatments and Chemical Peels)
Cosmetic procedures like laser therapy and chemical peels, if not correctly administered, may sometimes worsen PIH. Incorrect use of skin treatments, such as intense pulsed light (IPL) or aggressive peels, can cause further irritation. To minimise risk, consult a medical or aesthetic practitioner before undergoing these procedures.
Risk Factors of PIH
Certain individuals are more susceptible to developing PIH because of pre-existing conditions or environmental factors that increase their likelihood. Understanding these risk factors is important, as they highlight why some individuals may be more prone to PIH and can guide preventive measures.
1. Due to their naturally higher melanin baseline levels, darker skin tones are at a higher risk of developing PIH. In these skin types, inflammation triggers an overactive response in melanocytes (melanin-producing cells), leading to more intense and prolonged pigmentation.
2. Sun exposure is a significant contributor to PIH, as UV radiation stimulates melanocytes, darkening existing hyperpigmented spots and potentially triggering new ones. Studies show that consistent use of broad-spectrum sunscreen with SPF 30 or higher may help reduce the risk of further darkening, especially in individuals already prone to hyperpigmentation.
3. Genetic predisposition to inflammatory skin conditions, such as lichen planus and atopic dermatitis, increases the risk of developing PIH. Genetics influence how the skin responds to injury and inflammation, leading to increased melanin deposition during the healing process.
4. Persistent Inflammatory Skin Conditions: These conditions frequently cause irritation, and repeated flare-ups can result in PIH that may be more persistent. Managing these underlying skin conditions, through medical care or consistent skincare, may help lower the likelihood of PIH.
5. Improper handling of acne and skin injuries can worsen PIH. Picking or scratching at acne lesions can aggravate the inflammatory process, leading to more severe hyperpigmentation. Using aggressive skin treatments or applying products unsuitable for one’s skin type can also trigger or worsen PIH.
Symptoms of PIH
The symptoms of PIH appear as dark spots or discoloured patches on the skin after an inflammatory episode. These spots can vary in size, shape and colour depending on the severity of the original inflammation and the depth of the pigmentation.
Key symptoms include:
- Dark spots at the site of healed acne, eczema, or other skin injuries
- Persistent patches of discolouration, ranging from light brown to black (depending on the skin tone and depth of pigmentation).
- Worsening of pigmentation with further UV exposure
Types of Post-inflammatory Hyperpigmentation
Post-inflammatory hyperpigmentation (PIH) can be classified into three types based on the depth of melanin deposition in the skin: epidermal, dermal, and mixed. Understanding the classification can help explain why different approaches may be recommended for PIH.
1. Epidermal PIH
This type occurs when excess melanin is deposited in the epidermis, the outermost layer of the skin, and usually presents as brown or dark brown spots. Because the pigmentation is more superficial, epidermal PIH may be managed with topical agents such as hydroquinone, glycolic acid, salicylic acid, or azelaic acid.
2. Dermal PIH
Dermal PIH involves melanin deposition in the dermis, the layer beneath the epidermis. It typically appears as blue-grey or dark brown discolouration. Severe skin inflammation can cause melanin to be released into the deeper layers. Because of its depth, dermal PIH may not respond as well to topical agents, and some individuals may seek professional procedures such as laser therapy for management.
3. Mixed PIH
This condition combines epidermal and dermal pigmentation, presenting as patches that can appear brown, grey, or blue. Management may involve both topical treatments for superficial pigmentation and procedures such as laser therapy for deeper pigmentation.
Treatment Options for PIH
PIH may be managed through various methods, depending on the depth and extent of the pigmentation. Below are the primary categories often discussed in clinical and skincare contexts:
1. Topical Treatments
Topical agents are commonly used to manage PIH, particularly in its early stages. Common topical treatments include:
- Azelaic acid: Has anti-inflammatory properties and is used in the management of pigmentation and acne.
- Kojic acid: Inhibits melanin production and is used in the management of epidermal hyperpigmentation.
- Topical retinoids: Support skin cell turnover and may help improve pigmentation.
- Vitamin C: An antioxidant used to support skin health and protect against environmental stressors.
2. Medical and Dermatological Procedures
Medical procedures may sometimes be considered for more pronounced PIH. These include:
Chemical peels: Using glycolic or salicylic acid to exfoliate the skin’s surface, which may improve the appearance of epidermal PIH. Caution is advised in darker skin types as they may increase pigmentation risk.
Pico Laser treatments: Target pigmented skin cells and may help break down excess melanin. Some lasers can worsen pigmentation if used incorrectly, so professional guidance is important.
If you think you might have post-inflammatory hyperpigmentation, we recommend booking an appointment with Dr Kellyn Shiau to find a suitable treatment for your condition.
Preventing Post-inflammatory Hyperpigmentation
Prevention is always better than a cure. A consistent skincare routine and protective measures can help reduce the likelihood of developing PIH. This includes:
- Daily use of sunscreen with SPF 30 or higher. Reapply throughout the day for optimum sun protection.
- Avoid picking or scratching acne, eczema or other skin lesions
- Use gentle skincare products with anti-inflammatory ingredients
- Opt for gentle exfoliants like glycolic acid to promote cell turnover
Complications and Long-term Effects of PIH
If not properly treated or managed, post-inflammatory hyperpigmentation may last for months or even years, and in some cases can persist for longer periods. Sun exposure without protection may further darken the affected areas, making the discolouration more noticeable.
When to See a Medical Practitioner for PIH
It’s important to consult a medical practitioner when:
- The pigmentation persists for several months without improvement.
- Over-the-counter products do not appear to improve the pigmentation, or the discolouration seems to worsen.
- You’re uncertain about the cause of the pigmentation and need a diagnosis.
- The pigmentation is extensive or deep.
Book a consultation with Lux Medical Aesthetic Clinic to explore your treatment options and receive professional advice on managing PIH.
Conclusion
Managing post-inflammatory hyperpigmentation can take time, and outcomes vary depending on individual factors. Understanding the causes, risk factors, and treatment options is essential for managing and preventing PIH. If this condition persists, consulting a medical professional may provide helpful guidance and support.