Have you ever noticed tiny white bumps on your face that won’t go away, even with over-the-counter creams? They may look like whiteheads or pimples, but these bumps could be milia, a common and harmless skin condition.
Although they resemble comedones, milia form for very different reasons.
In this article, we’ll explain what milia are, the different types and causes, and how to manage them and prevent future occurrences.
What Are Milia?
Milia (also known as milk spots or oil seeds) are tiny white bumps that form when dead skin cells become trapped beneath the surface of the skin. These cysts often appear around the eyes and cheeks, but they can also develop on other parts of the body.
Types of Milia
Milia can be broadly classified into two main types:
- Primary Milia
- Secondary Milia
Primary Milia
Primary milia can be divided into several subtypes:
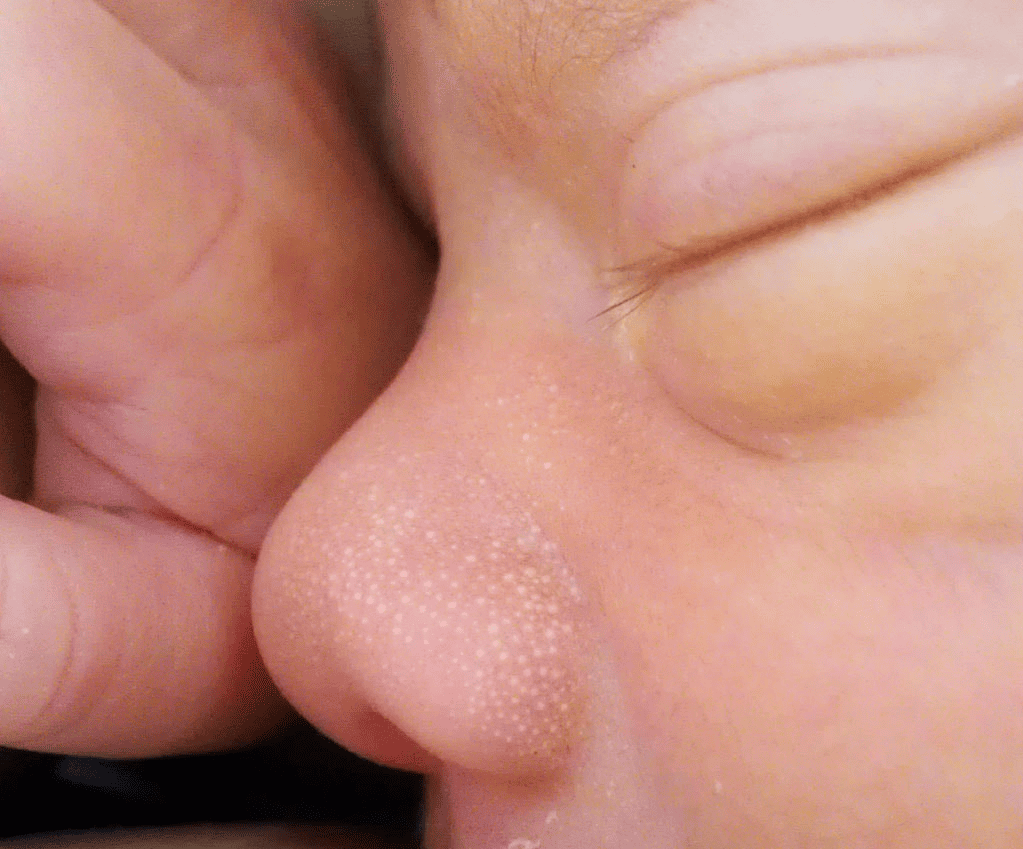
- Congenital milia. Commonly found in newborns, these milia appear at birth and typically resolve on their own within a few weeks. They are often referred to as ‘milk spots.’
- Benign primary milia. These can occur in children and adults and are usually spontaneous, often found on the face, particularly around the eyelids, cheeks and forehead.
- Milia en plaque. This type presents as an erythematous (red) plaque studded with multiple milia, which can vary in size.
- Nodular grouped milia. These appear as clusters of milia grouped closely together.
- Multiple eruptive milia. These appear suddenly and can be associated with underlying conditions or occur sporadically. It may last from a few weeks to several months.
- Genodermatosis-associated milia. Associated with genetic skin disorders like basal cell naevus syndrome and Rombo syndrome.
Secondary Milia
Secondary milia occur due to an underlying condition or trigger. Here are some of them:
- Disease-associated milia. These develop as a result of underlying skin diseases, such as epidermolysis bullosa or porphyria cutanea tarda.
- Medication-associated milia. This can occur due to the prolonged use of certain medications, particularly topical corticosteroids.
- Trauma-associated milia. Traumatic milia may develop following skin injuries, abrasions or burns.
| Type | Description | Common Locations |
|---|---|---|
| Congenital Milia | Present at birth, resolves spontaneously | Face, particularly nose |
| Benign Primary Milia | Occurs in children/adults, often spontaneous | Eyelids, cheeks, forehead |
| Milia en Plaque | Erythematous plaque with multiple milia | Various skin areas |
| Nodular Grouped Milia | Clusters of milia | Face, especially cheeks |
| Multiple Eruptive Milia | Sudden appearance, can be sporadic or associated with conditions | Face, upper trunk, groin |
| Genedermatosis-Associated Milia | Linked to genetic skin disorders | Varies based on the condition |
| Disease-Associated Milia | Develops from underlying skin diseases | Affected areas based on disease |
| Medication-Associated Milia | Result from certain medications | Affected areas based on treatment |
| Trauma-Associated Milia | Arises from skin injuries or trauma | Affected areas based on injury |
Causes of Milia
Several factors can contribute to the development of milia:
- Skin damage. Burns, blisters or trauma may result in secondary milia.
- Sun exposure. Prolonged sun exposure can cause the skin to thicken, making it harder for dead skin cells to shed properly.
- Using thick skincare products. Rich creams and ointments may clog pores and increase the likelihood of milia.
- Genetic factors. Certain inherited skin conditions may predispose individuals to milia.
- Trapped dead skin cells. When the skin’s natural exfoliation process is disrupted, dead cells can become trapped and form small cysts.
How to Identify Milia?
Milia are small, dome-shaped, white or yellowish bumps that appear on the skin. While they may resemble whiteheads, milia are not a type of acne and do not result from blocked pores. Instead, they are small cysts filled with keratin, a protein found in the skin.
Treatment Options for Milia
While milia are typically harmless and may resolve without treatment, some people choose to manage them for cosmetic reasons. Treatment options include the following:
1. Home Remedies and OTC Options
- Exfoliation techniques. Regular exfoliation helps remove dead skin cells and may reduce the risk of milia. Choose gentle exfoliants with ingredients like salicylic acid or glycolic acid, and begin with weekly use to avoid irritation.
- Retinoid gels and creams. Topical retinoids, including prescription-strength formulations, support cell turnover and may help prevent milia.
- Natural treatments. Remedies such as tea tree oil have anti-inflammatory properties and may assist in reducing milia. Always patch-test first to minimise the risk of irritation.
- For infants. In cases of neonatal milia, gently washing the baby’s face daily with warm water and mild soap may support natural resolution.
2. Extraction
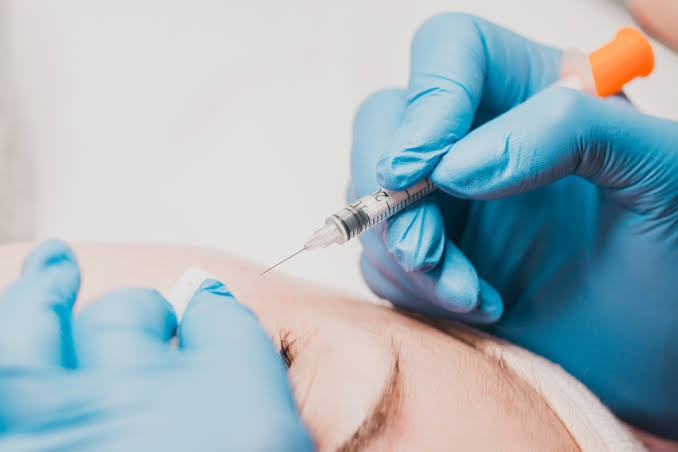
A medical practitioner may perform a technique known as manual extraction (de-roofing), where a sterile needle is used to gently puncture the milia and remove the keratin inside. This procedure should only be carried out by a qualified doctor to minimise the risk of complications.
3. Chemical Peels
Chemical peels use solutions like salicylic or glycolic acid to remove the skin’s outer layer and support the growth of new skin cells. This process may help reduce the visibility of milia.
4. Laser Resurfacing
Laser resurfacing can target and break down the keratin in milia. As with any cosmetic procedure, it’s important to speak with your doctor about potential risks before considering treatment..
5. Cryotherapy
Cryotherapy involves freezing milia using liquid nitrogen. This method may help manage their appearance, although temporary side effects such as swelling or blistering can occur.
How To Prevent Milia

Preventing milia involves adopting a skincare routine that supports skin health and helps minimise the risk of clogged pores. Here are some strategies that may help:
- Use non-comedogenic products. Choose skincare and makeup labelled as ‘non-comedogenic’, which means they’re formulated not to clog pores.
- Regular exfoliation. Incorporate gentle exfoliation to assist in removing dead skin cells, which may help in maintaining clear skin. Use exfoliating products containing alpha-hydroxy acids (AHAs) or beta-hydroxy acids (BHAs) a few times a week to keep the skin smooth and clear.
- Sun protection. Daily use of sunscreen (SPF 30 or higher) helps protect against UV damage, which can contribute to skin issues, including milia.
- Avoid thick skin creams. Heavy creams and oils may block pores. Opt for lightweight, breathable moisturisers instead.
- Hydration. Drink plenty of water throughout the day and use a moisturiser that suits your skin type to prevent dryness.
- Healthy diet. Eating a diet rich in vitamins and antioxidants can support your skin’s natural function.
- Get enough sleep. Quality sleep helps your body repair and maintain healthy skin. Aim for 7 to 9 hours each night
When to Seek Medical Advice
While milia are usually harmless, it is recommended to consult a doctor if:
- The milia persist despite home treatments.
- You notice changes in your skin’s texture or appearance.
- There are signs of inflammation, discomfort or fluid discharge, which may indicate an underlying issue.
Conclusion
Milia are common, harmless cysts that can appear at any age. They often resolve without intervention, but treatment options are available if they persist or cause concern. Maintaining a consistent skincare routine and sun protection may help prevent future occurrences.
If you have stubborn or persistent milia and would like professional medical advice, you can schedule a consultation with our doctor at Lux Medical Aesthetic Clinic



